For bunion and hammertoe sufferers, minimally invasive surgery is where the rubber meets the road.
Your feet are not tires. When they wear out, there is no replacing them. That being said, there are a number of painful podiatric conditions that can now be resolved with minimally invasive surgical procedures. It’s not like purchasing a brand-new set of Michelins, of course, but in many cases the end result is a smooth, bump-free “new tire” feel. Two of the most common foot deformities, in fact, are now correctable through a tiny, two-millimeter incision: hammertoe and bunions.
These specialized techniques have been around for a while, notes Dr. Aqsa Siddiqui, DPM, who performs the surgeries at Trinitas, however, “not many podiatrists have been trained in this procedure, so it’s not done at every hospital. It has an excellent track record and very high rate of success, so as a result, we’re seeing more and more podiatrists being trained now. Bunions and hammertoe are different deformities with different plans, of course. However, we are able to treat both with minimally invasive surgery and correct each of those problems.” Hammertoe is a biomechanical imbalance in the foot, due to an imbalance of muscles at the top and bottom of the foot, which causes contraction, typically at a toe’s middle joint. It is a democratic (small d) condition that breaks roughly 50-50 male/female, from all ages and walks of life, and from all nationalities and cultural backgrounds.
“We do see a fair number of young people with this condition,” Dr. Siddiqui says. “But typically my patients tend to have had the condition for a very long time—10, 20 even as long as 40 years—and it is causing constant pain and discomfort. They have already gone through other options, including trying different shoes with, say, a more spacious toe box, or orthotics or other conservative treatments, but nothing has helped.
Now they need something a bit more aggressive to correct the deformity.” Minimally invasive hammertoe correction involves a two-millimeter incision, through which podiatrists trained in this technique can go in and release the tendon and capsule, and then make small cuts to the bone to bring the toe up and reposition it properly, so it is no longer contracted. The surgery doesn’t involve any screws or plates; a special splinting of the toe is added within the post-operative dressing, and the bone naturally heals in the correct position within a few weeks. If a patient has multiple hammertoes, Dr. Siddiqui says she prefers to do one toe first and monitor how it responds to the procedure. “After that,” she says. “I will do the remaining ones together.”
The traditional surgery to correct hammertoe involves a recovery time up to six weeks for the toe to fully heal. The recovery time for the minimally invasive procedure, by contrast, is very quick. The patient leaves the hospital or surgical center in a walking boot (so there is no real down time) and the post-operative pain is minimal. A few days of Motrin usually quells any discomfort. The splint is removed after a week and, after two weeks, patients transition into a surgical shoe and can begin range-of-motion exercises. Between two and four weeks, they are fully healed. After that, they are good to slowly return to normal activities, including sports.
Dr. Siddiqui’s affiliation with Trinitas dates back a decade. After graduating from the New York College of Podiatric Medicine in 2012, she completed her three-year residency at TRMC. From there she accepted a wound-care and limb-salvage specialty fellowship before returning to Trinitas as an attending physician, working with residents and performing minimally invasive procedures. She began gravitating toward this specialty after her uncle, who lived in Pakistan, suffered a wound on his toe and ended up having to have it amputated. “I was studying here at the time,” she recalls, “and I think that was probably what got me interested in podiatry. I soon realized that it’s a great field. There is such a variety of things you can do to help people and make a difference…and still have your own personal life.”
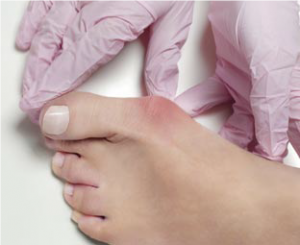
The recovery time for minimally invasive bunion correction is similar to that of the hammertoe procedure: You’re walking out of the hospital in a boot, which you’ll wear for a week or two, before transitioning into a shoe. Within four weeks, patients are fully healed. Whereas the causes of hammertoe tend to be consistent, not all bunions are created equal. The people limping into Dr. Siddiqui’s office may have developed bunions from a lifetime of repetitive stress or a genetic predisposition or as a result of flat feet—or some combination of causes. A mechanical imbalance of the muscles and tendons can also cause the deformity. Bunions are sometimes bilateral, but usually one foot is more severe than the other. What is unusual about the human foot that makes a bunion likely to form where it does, in the metatarsophalangeal joint of the big toe?
www.istockphoto.com
“The MTP joint is a very important joint that we use when we’re walking,” Dr. Siddiqui explains. “We roll off that joint. When there is an imbalance of the muscles, it can deviate that joint, causing that deformity. This in turn can cause damage to the cartilage in that area. Over time, the natural progression is that the big toe moves inward, overlapping or underlapping the second toe, or just squeezing against it. If the condition is not corrected, it progresses further and further into a severe deformity.” Traditional corrective surgery for bunions often involves opening up the entire toe and inserting plates and screws—frankly, to the layman it can sound a bit medieval.
Plus, there are occasional healing issues and complications and in some cases the pain and the bump can return after a certain amount of time. That is one reason bunion sufferers tend to opt for more conservative fixes, even before considering a minimally invasive procedure. Dr. Siddiqui is on board with this approach. “When a patient comes to me with pain in that joint, we like to begin with conservative treatments—injections, orthotics, physical therapy, comfortable shoes,” she says. “But if that isn’t helping, or if the pain returns, then surgery is an option.”
As with the hammertoe procedure, the bunion surgery involves a two-millimeter incision, through which a tiny drill can go in and shave off the bump, after which a cut can be made in the bone in such a way that it enables the surgeon to move the head of the metatarsal and reposition the toe. The technique involves a specific cut at a specific angle, which can be accomplished through the tiny incision. Can bunions come back? “Sometimes bunions do come back,” she says, “but from what I’ve seen—and this is echoed by other podiatrists who have been doing this for many years—compared to traditional surgeries, patients undergoing the minimally invasive procedure do really well in that regard.” So when is it time to kick the tires on bunion correction surgery? That’s an individual choice, of course.
And yes, Dr. Siddiqui is aware that there are folks out there who think they’ll just tough it out. “However, they should be aware that bunions don’t go away and tend to get worse,” she cautions. Indeed, the road to a more severe deformity can be paved with nerve damage, pain in the other toes, bursitis and eventually arthritis. Unfortunately, at the point when cartilage damage has progressed to where the joint doesn’t move anymore (hallux limitus), your options for a u-turn will likely be few and far between.
Editor’s Note: Dr. Aqsa Siddiqui, DPM, performs all of her minimally invasive procedures at Trinitas. She is in private practice in Carteret at The Foot Care Center of New Jersey, (908) 652–6077.