STOP THE CLOCK!
STOP THE CLOCK!
The first baby born in 2018 at Trinitas Regional Medical Center arrived at 11:17 am on January 2nd. Proud parents Rose Demosthene and Willick Joseph of Rahway pose with baby Isaac Joseph who measured 19.5 inches and weighed in at 6 pounds, 13 ounces. The nursing staff kept a long-standing tradition by gifting a complete layette to the New Year’s baby. Pictured are (left to right): Gabriella Moncayo, RN, Val Sivadasan, RN, Sabina Klos, RN and Mayra Via, RN.
 ACADEMIC EXCELLENCE
ACADEMIC EXCELLENCE
The Academy of Our Lady of Peace, New Providence has been awarded Blue Ribbon School status by the U.S. Department of Education based on its overall academic excellence.
The Blue Ribbon School award affirms the hard work of students, educators, families, and communities in creating a safe and welcoming school where students master challenging content. This prestigious award is given to a select number of private or public schools that exceed the criteria and represents exemplary teaching and learning. Only 229 public schools and 50 private schools out of the 133,000 public and 36,000 private schools in the USA had this honor bestowed on them. Pictured from left to right are Mr. Joel A. Castillo, Principal of the Academy of Our Lady of Peace, Mrs. Mary Rose Raleigh, Technology Teacher and Coordinator, and Father William A. Mahon, Pastor of Our Lady of Peace Church.
TRINITAS MINTS 71 NEW NURSES
Members of the Trinitas School of Nursing Class of January 2018 recite the Nightingale Pledge at the conclusion of convocation exercises held at St. Michael’s Church, Cranford. The 71 graduates are now are eligible to sit for the registered nurse licensing exam. Congratulations to the Trinitas School of Nursing’s 159th graduating class!
 MLB MVP’S
MLB MVP’S
MLB Residential Lending, LLC and Springfield Township officials held a rebranding ribbon-cutting ceremony last November. Officials conducting the ceremony were Springfield Township Mayor Diane Stampoulos and Springfield Township Deputy Mayor Maria Vasallo. MLB Residential Lending executive board includes Samuel Lamparello, Francis Lamparello, Justin M. Demola, Richard Doran, Marty Bronfman, and Daniel Gorczyca. MLB Residential Lending, LLC. is a community mortgage banker, founded under the belief that homeownership is the most viable means to secure a family’s financial future. The corporate office is located at 51 Commerce Street in Springfield.

GALLOPING TO THE RESCUE
Galloping Hill Inn and Galloping Hill Caterers in Union held a special event for the benefit of victims of Hurricanes Harvey and Irma. George Thomas, entrepreneur, philanthropist and owner of Galloping Hill, hosted the fundraiser. George (left) emigrated to the United States from Greece in 1951. He has been a leader in the food business and a generous supporter of local and national charities ever since.

LASSO-CUTTING ON 22 WEST
LongHorn Steakhouse recently celebrated the opening of its new Springfield location at 272 route 22 West. Joining managing partner Anthony Levy and his staff for this special “Lasso Cutting” was Springfield Mayor Diane Stampoulos, along with members of the Springfield Patriot Chamber of Commerce. The 5,869 sq. ft. restaurant, which seats over 200 guests, has created more than 90 new jobs for the community. Its design celebrates the natural beauty of the American West, with a wood-and-stone interior featuring contemporary artwork and sculpture. As part of its pre-opening training period, the restaurant hosted Friends & Family events with proceeds benefiting a local nonprofit. LongHorn Steakhouse (LongHornSteakhouse.com) prides itself on fresh, never frozen, expertly grilled and boldly seasoned steaks, prepared by a certified LongHorn Grill Master.
“Duck is Viana’s signature dish, and no matter the micro-season, he works what’s fresh and what’s purposeful into his nightly duck program.”
By Andy Clurfeld
When it comes to people with one-of-a-kind voices, New Jersey has given birth, or a place to work and live, or prominence to more than its share of singular talents.
Think Sinatra. Springsteen, of course —now a newly minted Broadway star. Count Basie, Whitney Houston, Queen Latifah, Sarah Vaughn, and Patti Smith. Then there are Einstein and Edison; Yogi Berra and Derek Jeter; Vince Lombardi and Bill Parcells. And also Annie Oakley, Shaq, “Marvelous” Marvin Hagler, Philip Roth and John McPhee, all peerless in their respective fields.
Now consider that Alice Waters, impresario of the ground-breaking Chez Panisse in Berkeley, CA, founder of the Edible Schoolyard initiatives and modern-day instigator of eating local and organic food, is from Chatham.
Yes, Alice Waters, whose influence on what and how we eat today is comparable to The Beatles’ influence on rock, is Jersey born and raised.
Time to take your medicine, Garden State denizens. Time to toss to the curb the cliches of New Jersey’s mass-produced culinary past promulgated by those intent on keeping original voices at bay while promoting the same old pizza and pork roll places, the overstuffed hoagies and subs and leaden bagels, as well as the ‘dogs, doughnuts and diners that give credence to out-of-town critics’ rants.
For there’s a new breed of chefs in New Jersey, and they are skilled, savvy and seeing things clearly now.
Leading the way are nationally regarded chefs, such as Dan Richer of Razza in Jersey City; Maricel Presilla of Cucharamama and Zafra in Hoboken, and Drew Araneo of Drew’s Bayshore Bistro in Keyport, as well as critically acclaimed voices with relatively new restaurants that include Ehren Ryan of Common Lot in Millburn; Greg Vassos of Brick Farm Tavern in Hopewell; and Randy Forrester of Osteria Radici in Allentown.
Factor in the wealth of ethnic restaurants that reflects the vibrant cultures and communities rooted in this, one of America’s most diverse states, adding both talent and a gastronomy that extends to all parts of the globe, and you have a collective table that groans glorious. It’s a simple mix of good ingredients and good people.

Photography courtesy of Heirloom Kitchen
It’s just what the doctor ordered as a prescription for eating in 2018.
David Viana, now chef-partner at Heirloom Kitchen in Old Bridge, could be the poster child for the vanguard born out of old guard.
He is Portuguese, raised in the traditions of the table, and took in the ways of professional cooking at some of the best restaurants in Europe, New York and New Jersey. Anthony Bucco, executive chef at the empire that is Crystal Springs Resorts in Sussex County, lauds Viana as the “most talented, gifted chef” he’s worked within a pro kitchen. Visionary chefs including Vassos and Ryan are honored to be part of collaborative dinners with Viana; young chefs, notably Jon Boot, now at Ryland Inn, Whitehouse Station, and Sean Yan, current pastry chef and assistant to Viana at Heirloom, are inspired by his food.
Because it’s unlike any other.
I’ve eaten a half-dozen dinners in as many months that either Viana created or collaborated on and find his voice to be, at present, the most original in the Garden State.
Viana starts with a main ingredient as his inspiration, be it duck or spring peas, apples or porcinis, scallops or cauliflower, and builds from there. His accents challenge and enlighten, yet they stop shy of being fussy. They are always artfully applied.

Photography courtesy of Heirloom Kitchen
Art on a plate scares me. I’ve seen and tasted too much artifice. Viana’s washes, pin-dots, and arcs of sauce, spears of vegetable, frothy poofs of concentrated herb and ringlets of leafy things never do anything but enhance the main element. The “art” supports, and shows, Viana’s control over a plate.
I’ve watched Viana in his open kitchen at Heirloom Kitchen—which is a restaurant three nights a week and a classroom other evenings—break down a duck: butcher the duck, score its fat, prep it till it’s ready to be called upon for a precise 40-minute stove-top sear that will star in a seasonal preparation. In the space of a few weeks late last year, there were two of note: johnnycakes and oatmeal, persimmon and delicata squash and a rush of pomegranate on a regular-dinner night in early December at Heirloom, and one with herbed wheat berries and granola, parsnips and date puree, coffee and pecans, and the unmistakable umami of maitakes with a squirt of duck jus at the venerable James Beard House in New York, where Viana was invited to cook dinner days before Christmas.
Duck is Viana’s signature dish, and no matter the micro season, he works what’s fresh and what’s purposeful into his nightly program. Viana’s regulars might have duck every month at Heirloom, without duplication.
They also might have pork belly with a bacon marmalade and loops of Vietnamese caramel, the richness of which is offset by thick-cut half-moons of celery and salty peanuts. They might have pork-smoked apple raviolo and come across on the plate a bacon-pine nut crumble there expressly to play off the pasta pockets with a slyly silky texture—as well as pivots of delicata squash and sweet potato and a splash of mustardy jus.
Scallops in cold weather will be appropriately accompanied by dug-up vegetables such as fingerling potatoes and carrots, both of which are roasted and—with the scallops —given a choice of playmates: almond-mint pesto, chestnut puree, and lemon-brown butter emulsion. The accent editing is pitch-perfect. Likewise, halibut will see kohlrabi smoked and pureed, chanterelles gently warmed, an egg yolk scented with truffle and mustard seeds pickled to give them added depth and a defiant edginess that the mild, dense, meaty fish appreciates.
Viana rises to the challenge of sides: Cauliflower gets a sultry-snappy lift from pomegranate molasses and mint pesto; kale is laced with duck confit and topped with a fried egg; Brussels sprouts are plied with a gastrique that bristles with mustard and then all’s calmed by the inherent sweetness of butter infused with, of all things, parsnip. You have to think: Sides? These are sides? They could comfort and cosset and fill in a bowl by themselves, eaten on a couch. Yes, they could. But they appear on Viana’s Heirloom menu, to be passed family-style at the table or counter, depending on where you sit.
If you are at Heirloom Kitchen, which is owned by Neilly Robinson, you will be seated (depending on your choice and the availability) at the chef’s counter, facing the stoves at which Viana cooks. A row back, there is another counter, also with a “view,” but without the same opportunity to watch, and converse with, the chef. Then there are tables of the regular dining-out sort—two-tops and four-tops, and a larger one for parties of perhaps 10.
I’m not forgetting dessert, made by Sean Yan to suit the Viana style. Lemongrass mousse, for instance, is backed by gingerbread and plated with white chocolate that’s been roasted and mint that’s been pulverized to the texture of dust. There’s the suspicion of bourbon in the mix, and a whiff of Asian pear.
But don’t count on repeats of anything you read here right now. In the world of a singular voice such as David Viana, yesterday is history to learn from, today provides a chance for change, and tomorrow is the opportunity to play out a dream deemed a privilege to share.
New Jersey, after all, thrives on its one-of-a-kinds
Heirloom Kitchen
3853 Route 516, Old Bridge • Phone: (732) 727.9444
Major credit cards accepted. Open Friday, Saturday, and Sunday for dinner and, generally, Tuesday, Wednesday and Thursday evenings for cooking classes. Menus change weekly and special collaborative dinners are planned seasonally. Visit www.heirloomkitchen.com to view schedules for classes as well as current menus. Reservations are required, and tables book early. Heirloom is a BYOB, but offers a small selection of wines from Domenica Winery for purchase on site.
Will your house become a virtual doctor’s office?
by Caleb MaClean
In November 2017, the Food and Drug Administration approved Abilify MyCite, the first “digital” pill. The pill, made of silicon, magnesium, and copper, contains a sensor no bigger than a grain of sand. It communicates with a patch worn by the patient, which then trans its medical data to a smartphone app, which in turn uploads it to a database that’s accessible to a patient’s doctor (and also family members). The sensor is activated when it interacts with stomach acid and transmits the time the pill is taken, as well as the dosage.
Abilify is a medication that treats bipolar disorder, depression, and schizophrenia, all of which demand that a patient stay on schedule with medication. The digital pill makes for easy monitoring by a third party. Although there are some inherent privacy issues that will probably need to be worked out, the big picture for healthcare is big indeed: By some estimates, the improper or unnecessary use of medication costs the industry $200 billion annually. To wrap your head around that number, consider that the total amount of property taxes paid by New Jersey homeowners in 2018 will probably be about $30 billion. With that much money on the table, you’d better believe a flood of digital pills is on the horizon.

www.istockphoto.com
This is just the beginning of a revolution that will move more and more elements of traditional medicine into the home—to the point where, one day, more doctoring will be done through digital housecalls than in medical practices. Which is why, in 2017, the FDA created a new unit devoted entirely to digital health.
It is being staffed with engineers well-versed in software development and artificial intelligence, who are able to deal with the steadily growing flow of medical technologies that require FDA approval. While certain parts of the federal government maneuver at a snail’s pace, the FDA is changing its culture to deal with the day in the not-too-distant future when machines will be monitoring and regulating a huge part of the healthcare industry. The FDA has long considered medical “apps” outside of its purview and thus the vast majority are currently unregulated. As more and more traditional medicine moves out of the doctor’s office and into our bedrooms and living rooms, that will need to change. And soon, for all of our sakes.
The digital pill is, in its own way, a forerunner of how our homes will become part of the pharmaceutical industry Within a few years, 3-D printers will be integrated into millions of American homes, plugged right into our smartphones and laptops. At the moment they are novelty items, but the capability to “print” pills on an as-needed basis may make them as common as home-testing machines for blood glucose or coagulation levels. Besides the cost savings and the convenience factor, this technology could also create pill shapes that release medications at different rates. For patients who need medications “tweaked” regularly, 3-D printers would be a godsend.
DOCTOR, DOCTOR
The digital housecall will be commonplace years before the printed pill. Ask people who work in the tech industry and they’ll tell you it can’t come soon enough. Besides the new FDA unit, there is already a trade organization promoting digital medical consultations, the American Telemedicine Association. Several insurance carriers either cover, or say they plan to cover, webcam exams and consultations. At the moment, digital housecalls are being conducted primarily in rural areas, via smartphone and Skype. The visual component is key; according to health insurance giant Aetna, the error rate is one-fifth that of voice-only doctor consultations.
Actually, the digital housecall is nothing new. It’s around 10 years
The initial driver was distance. In places like Maine, where a single hospital may cover hundreds (or even thousands) of square miles, keeping patients off the road is a huge priority. Maine, in fact, was one of the proving grounds for telemedicine. Doctors there used telemedicine in a wide range of situations, including burn and trauma cases, where victims had to be helicoptered in for emergency treatment. They found they could begin “treating” those patients en route or, in some cases, on the scene.

www.istockphoto.com
Going forward, the driver of telemedicine will be cost (or more to the point cost savings). A doctor can see more patients digitally than in an office, which creates money saving— and money-making—efficiencies. Patients, on the other hand, benefit financially, too. They save time and money by staying at home or at work during a medical consultation. The necessity of hands-on contact is certainly an issue, but as more “connected” monitors and diagnostic devices come online, the need for doctors and/or medical staff to be in the same physical space as their patients will decline. Right now, insurers estimate that only about 20 percent of visits to a GP actually require a GP. Think about your last visit to the doctor’s office: How much physical contact did you have with your doctor? How much of your check-up was off-loaded to a nurse of staff member? Much of what a doctor does is ask a series of questions and listen carefully to your answers—which can be done on a screen.
So how exactly will this work?
Based on what already works in the places that telemedicine has a track record, it’s not difficult to paint a realistic picture. Patients will register online with the primary care physician or medical group that currently serves them, or possibly with a hospital center such as Trinitas. Though the particulars are likely to vary somewhat from insurance plan to insurance plan, patients will make appointments to interact with doctors (or other healthcare workers) in a space in their house or apartment where they can see and hear each other, and where the patients have access to biometric devices that plug into a smartphone or computer. Given that most of the equipment in a doctor’s office—and for that matter in a hospital—already “talks” to computers, there is no reason why simpler, cheaper home versions couldn’t be made available to patients with chronic illnesses or other conditions that require periodic monitoring. Right now, people with artificial heart valves already test their own blood weekly in order to tweak their Warfarin dosage (a famously moving target) and report PT/INR levels to their cardiologists. Five years ago, the home equipment was expensive and cumbersome; most patients had to drive to a lab to get their blood drawn and tested. Now the device is the size of a Game Boy. Five years from now, or perhaps much sooner, the next generation of these monitors will feed data directly into the cardiologist’s computer.
As hospitals cross the digital divide, they are likely to find telemedicine a force-multiplier, as well as a profit center— especially if they offer distinct specialties. For example, there are patients who travel many hours multiple times a week from surrounding states to see the wound-healing specialists at Trinitas. Not all of those trips are related to procedures performed on-site; a fair number are progress-checks and dressing changes that could conceivably be conducted without a patient leaving the home.
DIGITAL DOC-IN-A-BOX

www.istockphoto.com
If you think about it, the reduced need to physically visit a doctor’s office cuts both ways—if the patient can stay at home, why not the doctor? Your digital housecall may be conducted by a physician working remotely, too—perhaps from his or her own home or home-office. There are, in fact, thousands of doctors who already work this way. Many are part of existing telemedicine groups. These companies treat hundreds of thousands of patients and are constantly tweaking how their platforms deliver healthcare to under-served or isolated communities.
At the moment they are kind of like virtual “Doc-in-a- Boxes,” bringing basic diagnostic services into homes. But make no mistake about it…they have their sights set on a bigger piece of the pie.
MDLive, which began offering digital housecalls almost a decade ago, recently added dermatology to its roster of services. It did so by partnering with an existing company called Iagnosis, an online skincare company that developed a platform called DermatologistOnCall. “Teledermatology” (they need to work on that name, by the way) makes sense on a lot of levels.
First, it is a very visual branch of medicine, from training to practice, so it lends itself to a camera and screen. Second, how long do you have to wait to see a dermatologist on your current insurance plan? California-based SnapMD, a relative newcomer to the industry, just launched an app that enables Spanish-speaking patients to communicate with doctors who don’t speak Spanish, and vice-versa. Wall Street is watching companies like these very carefully, trying to divine where the “tipping point” is for the industry. Some believe it is coming in the next year or two.
HOME, SMART HOME
Homebuilders also are paying close attention to this space. They are already partnering with tech innovators on ways to make their homes “smarter” and recognize that, as Baby Boomers age, telemedicine will become a part of their lives. Some builders, in fact, may be thinking really big: Not only will future housing units double as doctors’ offices, by incorporating medical hardware and software, they may double as “doctors,”
The first group to break ground on this idea was a research team at the University of Rochester. Back in the early 2000’s, they initiated a project called the Smart Medical Home. Its goal was to develop interactive technology for home healthcare. It brought together doctors and engineers from the university, Rochester Medical Center and the Center for Future Health. Over the next few years they designed living spaces that actively assisted patients with dementia and Parkinson’s. A Personal Medical Monitor was built into one of the walls. It featured an avatar that interacted with residents and answered questions about medication and symptoms of illness. Sensors located around the structure were designed to monitor the resident and could alert his or her doctor if it detected a change in vital signs.

www.istockphoto.com
The home-as-doctor concept has continued to pick up steam in the ensuing years, as computing power and artificial intelligence have doubled, doubled again and doubled again. In 2015, a story in Healthcare IT News on smart medical homes reviewed a number of machine-tomachine (M2M) health devices in development for home use, including monitors built into footwear that can detect a limp or shuffle that may be a symptom of a more serious illness—and transmit this information through the home. In 2017, the same Center for Future Health in Rochester received funding for the development of tiny, wearable health monitors that transmit data to a base station in the home. The monitor incorporates “predictive” health software that can spot developing health issues, manage daily routines and intervene in the case of an emergency. The system constantly evaluates activities, motion, breathing, the sound of the wearer’s voice and how they all intersect.
It is not just the home and health industries that are working toward this goal. At the 2018 Consumer Electronics Show in Las Vegas, CNET held a forum entitled The Invisible Doctor. A panel of tech, medical and insurance industry experts explained how everyday items—from smartphones to home appliances—could potentially be part of a health-monitoring network keeping us connected to our doctors through our smart homes.
Some things, however, simply must be done in a doctor’s office or hospital setting. So the digital housecall will never replace brick-and-mortar medicine. That’s not the idea, anyway. The goal is to make the “front line” of healthcare more time- and cost-efficient and to make doctors more accessible to more people in more places.
Just as important is the byproduct of that goal: To give doctors access to patients before small problems become big ones.
NATURAL DISASTERS
Telemedicine has the potential to play a major role in disaster relief efforts. One of the first things that happens in stricken areas is the collapse of the healthcare infrastructure. Hospitals may keep their doors open and restore power during a crisis—they are built to do this— but are unlikely to be able to cope with the ensuing spike in demand from scores of the sick and injured. In these cases, access to virtual doctors and diagnostic services would prove invaluable in coping with the patient surge at brick-and-mortal hospitals. Down the road, these relationships could conceivably extend to remote surgical procedures, performed by surgeons in daVinci pods like the ones at Trinitas, working on patients in OR’s thousands of miles away.
 OLD SCHOOL
OLD SCHOOL
One of the great debates around digital doctor visits is how easily older patients will take to the new paradigm. The implication is that individuals over a certain age are intimidated by technology, or are total Luddites. That may be, but balanced against the comfort level of seeing your own doctor in your own home, it may be less of an issue than critics claim. As home/medical technology advances it will, by definition, become simpler to use, with fewer buttons to push and procedures to follow. You can already get a TV remote you can talk to…biometric devices that follow voice commands can’t be too far behind.
TELEMEDICINE HURDLES
For digital medicine to become fully integrated into the healthcare system, two major challenges will have to be continually addressed. While the hardware end of the business will become faster, better and cheaper, the software may struggle to keep up—and not just the software that runs diagnostic tools. As is currently the case with in-office visits, everything a doctor does will have to be coded and entered into a database used for billing, coverage eligibility, deductibles, referrals, and reimbursements. If you’ve ever peeked behind your doctor’s reception desk at the wall of paper files, you know how much information is kept on patients. Which bring us to the second major hurdle: With all that information digitized for digital doctor visits, just how safe will it be? Federal HIPAA laws create high standards for record-keeping, but can HIPAA regulations anticipate the legal and technical loopholes that digital medicine will almost certainly create?
In town as the seasons change…

Cameron Yee
February 16
Jeff Dunham: Passively Aggressively
Prudential Center 7:00 pm
Comedy superstar Jeff Dunham brings his cast of ill-behaved characters to The Rock for his Passively Aggressively tour. Fan favorites, such as Bubba J and Peanut, consider what a new member to their dysfunctional family could mean.
February 16-24
Pippin
Kean Stage
(See web site for showtimes)
Pippin’s Leading Player tells the powerful story of his travels with a troupe of talented actors. Music, song, and dance weave a narrative of selfishness, deceitful first impressions, and the power of redemption.
 February 17-18
February 17-18
Men are from Mars, Women are from Venus Live!
NJPAC/Victoria Theater
(See web site for showtimes)
For more than two decades, John Gray’s hilarious Men Are From Mars, Women Are From Venus guide to the battle of the sexes has remained an audience favorite.

Joe Satriani
February 18
G3 2018: Joe Satriani, John Pertucci, Phil Collen
NJPAC 7:00 pm
The G3 2018 tour features Satriani and fellow six-string legends Pertucci and Collen in an action-packed, live-wire celebration of guitar wizardry.
 February 18
February 18
Hot Latin Nights with the Mambo Kings:
New Jersey Symphony Orchestra
State Theater 3:00 pm
Bringing some serious heat, The Mambo Kings celebrate the sizzling, jazz-infused music of Latin America and the United States.

Amazon.com
February 23
Art of Rap: The History of Hip Hop Tour with Bone Thugs-N-Harmony, EPMD, N.O.R.E., Big Daddy Kane, Onyx, MR. Cheeks, Brand Nubian, and Roxanne Shanté
NJPAC 8:00 pm
This electrifying concert features some of the most influential Hip Hop artists of today—and back in the day. It’s a celebration of the far reach of rap and the amazing stories of its unforgettable artists.
 February 24
February 24
Jon Secada
UCPAC Main Stage 8:00 pm
Grammy Award-winning artist and songwriter Jon Secada, acclaimed for his romantic sound, takes the Main Stage in Rahway with his soulful and melodic voice.
February 24
Brahms’ First Symphony: New Jersey Symphony Orchestra
State Theater 8:00 pm
Rune Bergmann conducts mezzo-soprano Marianne Beate Kielland and the New Jersey Symphony Orchestra in Brahms’ First Symphony, a masterwork for all time.

The Duprees
March 3
Golden Oldies Spectacular
State Theater 7:00 pm
An evening of beloved oldies in New Brunswick! Featuring classics like The Duprees’
“You Belong to Me,” The Marcels’ “Blue Moon” and many more.
March 4
Staatskapelle Weimar
State Theater 3:00 pm
Founded in 1491, the Staatskapelle Weimar is one of the oldest and most illustrious orchestras in the world. It’s the organization’s first North American tour to present three of Beethoven’s greatest works.

Thefallofitall
March 9
Colin Quinn: One in Every Crowd
NJPAC/Victoria Theater 7:00 pm
Quinn’s rough-hewn urban humor has entertained MTV, Saturday Night Live, Comedy Central, and Broadway audiences. He comes to Newark with an entirely new show.

PeterPan23
March 9
Kid Rock: Greatest Show on Earth Tour 2018
Prudential Center 7:30 pm
Kid Rock brings his The Greatest Show on Earth Tour to The Rock—to promote his new album, Sweet Southern Sugar
March 11
Zhang Conducts Tchaikovsky: New Jersey Symphony Orchestra
State Theater 3:00 pm
Acclaimed conductor Xian Zhang conducts the New Jersey Symphony Orchestra in Tchaikovsky’s Sleeping Beauty and Francesca da Rimini, Danielpour’s Carnival of the Ancients, and Haydn’s Sinfonia Concertante.

NJPAC
March 16
Los Tigres del Norte
NJPAC 8:00 pm
One of the most influential Latin music groups of all time, Grammy-Award winning Los Tigres perform high-energy norteño music that celebrates the vibrant culture of Mexico.

State Theater
March 17
Dublin Irish Dance
State Theater 8:00 pm
Stepping Out offers an extravaganza of sights and sounds from the Dublin Irish Dance company. The troupe of accomplished step-dancers and musicians explores Celtic history and culture.

State Theater
March 18
Academy of St. Martin in the Fields with Joshua Bell
NJPAC 3:00 pm
Known as one of the greatest American violinists of his time, Bell has recently become one of the world’s most accomplished conductors. He now leads the Academy of St. Martin in the Fields.
FOR the KIDS
 February 9-10
February 9-10
Rogers & Hammerstein’s Cinderella
State Theater
(See web site for show times)
February 10
Beauty & the Beast
Kean Stage 3:00 pm
February 10
Year of the Dog: The Nai Chen Dance Company
NJPAC/Victoria Theater 2:00 & 7:00 pm
February 19
Mr. Popper’s Penguins
State Theater 10:00 am, 12:30 & 3:00 pm
March 3
Moon Mouse: A Space Odyssey
NJPAC/Victoria Theater 2:00 pm
March 3
Harry Potter and the Prisoner of Azkaban in Concert
NJPAC 2:00 & 7:30 pm
 March 15-18
March 15-18
Marvel Universe Live! Age of Heroes
Prudential Center
(See web site for showtimes)
March 17
Popovich Comedy Pet Theater
NJPAC/Victoria Theater 1:00 & 5:00 pm

YouTube
March 18–19
Mummenschanz
State Theater 7:00 pm

Sibuachu
March 20
Judas Priest
Prudential Center 7:00 pm
One of heavy metal’s iconic acts hits the road to support the new Firepower album. The lineup features Rob Halford, Glenn Tipton, Richie Faulkner, Ian Hill, and Scott Travis.

Sibuachu
March 21
Demi Lovato & DJ Khaled
Prudential Center 7:30 pm
Grammy-nominated, multiplatinum singer Demi Lovato brings her tour to North America timed with the release of her critically acclaimed album Tell Me You Love Me. She is joined by special guest DJ Khaled.
 March 23
March 23
National Symphony Orchestra of Cuba
NJPAC 8:00 pm
Conducted by Enrique Pérez-Mesa—with guest pianist Yekwon Sunwoo—the orchestra makes its NJPAC debut with a Latin-flavored and dance-inspired program.
March 23-25
Motown the Musical
State Theater (Check web site for showtimes)
Celebrate the music that transformed America and the story of Berry Gordy’s journey from featherweight boxer to heavyweight music mogul.
March 29-April 29
The Sting: A New Musical
Paper Mill Playhouse (Check web site for showtimes)
Based on the 1973 Academy Award-winning film, The Sting, this musical tells the story of two con men who plot to sabotage a corrupt racketeer in Depression Era Chicago.
April 4-7
Comedy of (Jersey) Errors
Kean Stage (Check web site for showtimes)
This version of Shakespeare’s Comedy of Errors is filled with madcap characters, adventure, and everything “Jersey Shore,” as long-lost twins cross paths on the Garden State’s beloved boardwalk.

Louise Palanker
April 5-6
Frankie Valli and The Four Seasons
NJPAC/Victoria Theater 8:00 pm
Spend an evening with Rock and Roll Hall of Famer Frankie Valli, performing classic Four Seasons hits like “Big Girls Don’t Cry,” “Rag Doll,” and many more.

Liliane Callegari
April 6
Lorde
Prudential Center 7:00 pm
Grammy Award-winning artist Lorde takes the stage with special guests Run the Jewels and Mitski to support her new album UPROXX.
April 7
The Sleeping Beauty: Russian National Ballet
NJPAC 8:00 pm
This sumptuous company brings a traditional staging of the classic fairy tale to NJPAC with stunning precision and beauty.

World Economic Forum
April 8
The Silk Road Ensemble with Yo-Yo Ma
NJPAC 3:00 pm
Cellist Yo-Yo Ma returns to Newark with his ensemble to celebrate music that crisscrosses centuries, continents and cultures. Last performed in 1998, this program embraces the artistic traditions of more than 20 countries.

Dwight McCann
April 13
Johnny Mathis
NJPAC 8:00 pm
Music legend Johnny Mathis returns to NJPAC for another pitch-perfect performance of his greatest hits.
April 14
P!nk: Beautiful Trauma World Tour 2018
Prudential Center 8:00 pm
International pop icon P!nk brings her high-energy and imaginative performance to the Prudential Center to promote her highly anticipated seventh album, Beautiful Trauma.

Upper Case Editorial
April 15
Jason Alexander: The Broadway Boy
New Jersey Symphony Orchestra
State Theater 3:00 pm
Long before becoming inhabiting the beloved comic character George Costanza on Seinfeld, Alexander made his career as a Tony-winning Broadway song-and-dance man. Alexander returns to his roots for an afternoon of music, laughter, and fun.
Editor’s Note: This overview of local entertainment, curated by Rachel Stewart, is just a taste of our area’s overall performance picture. For full listings, log onto the following web sites:
Kean Stage • keanstage.com
Paper Mill Playhouse • papermill.org
State Theater • stnj.org
NJPAC • njpac.org
Prudential Center • prucenter.com
Union Country Performing Arts Center & Hamilton Stage • ucpac.org
New technologies have changed the landscape for pulmonologists.
By Mark Stewart
A lot of people joke that you can’t tell doctors anything. Don’t tell that to Dr. Carlos Remolina. And know that, when it comes to early detection of lung cancer, it’s no joking matter. On a Monday evening back in December, the Chief of the Pulmonary Division addressed the assembled Department of Medicine at Trinitas on how and when to employ the dramatic technological advances in his area of medicine. Much of his time was devoted to reviewing the fine points of Bronchial Navigation, a new way to detect the minute, shadowy nodules that could be the beginning of lung cancer.
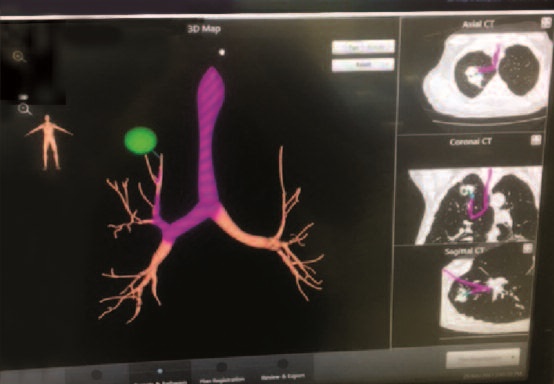
“I presented several cases we have encountered here at Trinitas, one in which the nodule was as small as nine-by eleven millimeters,” says Dr. Remolina. “We were able to identify the nodule and use Navigational Bronchostomy to reach it and do a biopsy. The patient did have lung cancer, but because we detected the disease in its earliest stage, we were able to perform a resection and save that patient’s life.”
 Where lung cancer is concerned, it is all about early detection. The 10-year survival rate for patients diagnosed in Stage 1 or 2 is 88 percent; in Stage 3 and 4, the five-year survival rate is just 17 percent. In his presentation, Dr. Remolina encouraged his fellow doctors to be more proactive when it comes to using the new technology. Medicare actually covers lung screening for “30-pack smokers” ages 55 and over, and Trinitas has a superb Lung Screening Program that employs a low-dose CT scan.
Where lung cancer is concerned, it is all about early detection. The 10-year survival rate for patients diagnosed in Stage 1 or 2 is 88 percent; in Stage 3 and 4, the five-year survival rate is just 17 percent. In his presentation, Dr. Remolina encouraged his fellow doctors to be more proactive when it comes to using the new technology. Medicare actually covers lung screening for “30-pack smokers” ages 55 and over, and Trinitas has a superb Lung Screening Program that employs a low-dose CT scan.
“Our program is not used as aggressively as it should be,” says Dr. Remolina, who adds that lung screening needs to become more ingrained in the medical community. Not only is it potentially a matter of life and death, he points out, it could soon be a matter of liability. When a woman goes to a doctor and that doctor doesn’t order a mammogram, the doctor could be liable if she develops breast cancer. The same could be true for a doctor who fails to refer an older ex-smoker for screening and a full workup if, years later the diagnosis is Stage 4 lung cancer.
HOW IT WORKS
Navigational Bronchostomy employs electromagnetic fields that create “GPS” to tumors when they are very small, so they can be reached and biopsied. A computer program generates a 3-D map that pinpoints the location of the tiniest tumors, and shows the twists and turns along the way. Prior to this technology, the diagnostic options faced by patients at risk for lung cancer were limited. They included traditional bronchoscopy, which often could not reach the area of concern or an invasive surgical procedure. Needle biopsies sometimes didn’t get to the target and came with a significant risk of pneumothorax, more commonly known as a collapsed lung.
“Another option was watching and waiting,” Dr. Remolina recalls. “When a nodule got big enough, you’d go after it. By that point, of course, the tumor had grown.”
The new technology, he adds, reduced the risk of lung collapse from a range of 18 to 30 percent to just 2 or 3 percent. What are some of the first signs that suggest someone should get a screening?
“An unexplained cough, especially one that brings up a small amount of blood, would be a major area of concern,” Dr. Remolina says. “Unexplained weight loss is something to watch for, too.”
These symptoms are much more likely to occur in smokers, but lung cancer can also affect people who never smoked a cigarette in their lives. Unfortunately, those individuals don’t meet the criteria for low-dose CT scans at the moment.
Another procedure that has come online in recent years is Endobronchial Ultrasound, or EBUS, which Dr. Remolina also says is a game-changer: “Before EBUS, you had to send a patient to a thoracic surgeon for a procedure on a lymph node. Now it can be done as an outpatient procedure.”
Dr. Remolina maintains that advances such as Navigational Bronchostomy and Endobronchial Ultrasound have changed the landscape of pulmonology. His goal is to encourage more physicians to embrace these procedures. It’s a matter of smart medicine and, potentially, life and death.
LOW DOSE/BIG RESULTS
The Trinitas lung screening program has been up and running for 18 months and, in that time, has already demonstrated its life-saving potential. The low-dose, non-invasive CT scan—which takes less than a minute—has detected tiny, early-stage tumors in dozens of patients, dramatically altering outcomes for those individuals. Lung cancer kills more people in this country than breast, colon and prostate cancer. Combined. The Trinitas screenings involve only a quarter of the radiation of traditional CT scans. For more information on the Lung Screening Program at Trinitas call (908) 994-5051.
 Carlos Remolina, MD, FCCP, PA
Carlos Remolina, MD, FCCP, PA
Chief/Pulmonary Division,
Trinitas Regional Medical Center
Director, Care One LTACH
908.241.2030
My unlikely encounter with a silent epidemic.
By Dree Andrea
Twenty-five years had passed since my last visit to a doctor’s office. Which is why, in 2016, finding myself in a constant state of fear and paranoia, the thought of doing so never even crossed my mind. It happened practically overnight. I grew increasingly afraid of leaving my house. My dreams were so vivid that I started to confuse nightmares with reality. In order to (literally) save the day, my subconscious ordered the insomnia that followed. After five days without sleep, however, I became terrified of my fellow human beings. I had always considered myself a grounded, healthy, joyous person who met all the responsibilities that come with living life. I did my best to remain calm and logical, but I was also aware that my emotions were on the verge of total collapse, and would get the better of me sooner rather than later.
 A traumatic experience with the medical community early on in my life in Amsterdam (where I was born and raised) had motivated me to study a variety of holistic healing modalities after I came to America. When health issues arose that I could not address myself, I had worked successfully with a chiropractor and an acupuncturist, but never a traditional GP. Once, while experiencing severe pain after being clipped by a hit-and-run driver, a colleague convinced me to take an aspirin. It made me so sick that I decided to never touch over-the-counter medication again. Arnica gel for sprained ankles and Old Indian Wild Cherry bark for severe coughs were as far as I would go, no matter how grave the situation. I was a happy, healthy artist and documentary filmmaker living in the States for over 20 years when I began to “lose my mind.”
A traumatic experience with the medical community early on in my life in Amsterdam (where I was born and raised) had motivated me to study a variety of holistic healing modalities after I came to America. When health issues arose that I could not address myself, I had worked successfully with a chiropractor and an acupuncturist, but never a traditional GP. Once, while experiencing severe pain after being clipped by a hit-and-run driver, a colleague convinced me to take an aspirin. It made me so sick that I decided to never touch over-the-counter medication again. Arnica gel for sprained ankles and Old Indian Wild Cherry bark for severe coughs were as far as I would go, no matter how grave the situation. I was a happy, healthy artist and documentary filmmaker living in the States for over 20 years when I began to “lose my mind.”
Of course, my American friends had long questioned my sanity, albeit jokingly.

www.istockphoto.com
My belief that diet is the key to physical, emotional and mental health has made me an object of curiosity. On occasion, I have been called stubborn or even stupid for living my holistic lifestyle. I ate solely organic food and avoided sugar, coffee, and alcohol. I also exercised and practiced yoga and mindfulness. I learned through my own success—and as a graduate of the Natural Gourmet Institute in New York—that staying healthy (and doctor-free) takes a lot of time and attention, willpower and discipline. Eventually, I started coaching others—acquainting each client with the tools and techniques necessary to discover the lifestyle that worked best. In some cases, I imparted knowledge I had acquired in other areas, like Reiki, a form of hands-on healing developed in Japan. I also believed the key to balance and happiness was connecting to your creative self, whether through journaling, painting, cooking, or some other passion. I held art and cooking classes, as well as dream workshops. I was a Jack-of-all-trades with a stack of certificates, but no conventional degree. Even so, as the years went by, with a track record of positive reactions and referrals, I was satisfied that my degree in Life Experience was an acceptable alternative.
On paper, I was the last person who should have been swept away by this tsunami of negative energy. Over the previous seven years, I had dealt successfully with a series of unexpected stressful events, including a separation, the passing of a few dear friends, and working with a psychotic life-coaching client who turned out to be far more dangerous than I had been willing to admit while working with him. Also, I had recently made a major quality-of-life decision that I considered to be very positive. After two decades in a New York rental apartment, I had initiated a project that opened up the opportunity to purchase a fairytale weekend home in New Jersey, the perfect place to one day create a coaching practice and writer’s den. I knew the city eventually would become too demanding for the sensitive soul that—at age 50—I recognize that I am.
Most of my life I had been told to “not be so sensitive” and to “get over myself.” In 2010, however, I learned from one of the professionals with whom I worked that I am indeed an unusually (physically and emotionally) sensitive individual. Which is to say that I need a little less stimulus and a little more nature than the average person. So the location of the house—in a national historic district, with unpaved roads winding up and around a hillside overlooking the ocean, an absence of streetlights, friendly neighbors and lots of wildlife—was a dream come true. As technology has rushed forward, time has barely moved there. I saw it as a new phase in life. I hoped to find the community I missed in New York and I intended to practice what I preached, in order to eventually obtain my “Master’s” in Life Experience. Even if the unsettling experience with the aforementioned coaching client had taken place in this house, when my emotions started to unravel, I still felt peaceful there, protected by nature, thankful for this safe haven.
One day in November 2016, I entered my home and something seemed terribly wrong. Panic struck me like a bolt of lightning. I ran outside, finding myself standing under a full moon, in freezing weather, without a coat. The chill I felt was not from the cold. The house was haunted. The hill was haunted. “You’re going crazy,” I said out loud, trying to compose myself. “No one knows about it yet. And you better make sure they don’t find out!” Hearing my own words grounded me. I would rather die than get locked away in a psych ward. Thinking of the birds, crickets and squirrels with whom I cohabitate in this magical place, I took off my shoes and connected with Mother Earth. I had trained with shamans in Peru a decade earlier; Patcha Mama would come to my rescue, I just knew it. I had never felt so grateful in my life. “I’m no lunatic,” I declared, looking up to the huge, bright full moon.

www.istockphoto.com
However, in the ensuing months, I grew more and more tired. I started to lose my ability to concentrate or focus. I had completely lost my grip. I reacted to everything like a deer in the headlights. My self-confidence crumbled. It was like living outside of a box made of unbreakable, soundproof, see-through glass looking in, but at the same time being locked up inside that very same box, reaching out to myself for help. Neither of us could find a door to even knock on. I was a documentary filmmaker trapped in a horror movie.
Deep down inside, I sensed that I had just lost my way. I never lost my identity. Yet it was hard to continue to believe in myself as more and more people who had known me for a long time, when confronted with my personality change, seemed to be looking to create a little distance. I kept hearing that I appeared pretty healthy and, therefore, it could not really be that bad. Some suggested antidepressants, others that I get a dog. In my world, those were not solutions. I just wanted people to be part of my life again; I was desperately looking for support from humans, not animals. A caring neighbor who had attended and appreciated my dream workshops—and who was familiar with my diet— offered up another idea. She is all about finding balance, but seeks it in different places, in different ways than I do.

Dree AndreaShe suggested I might have a vitamin deficiency. The one thing I had not considered or tested were the levels of my vitamins, minerals, and hormones.
So it came to pass that I found myself in an examination room for the first time since the early 1990s. I was terrified of how an M.D. might approach whatever the outcome of the lab work would be but fortunately managed to find a doctor who was open to holistic modalities. It turned out that I did indeed have severe vitamin deficiencies—caused by long-term stress, which had taken its toll on both my sleep as well as my digestive system. Due to malabsorption, she said, I was dangerously low in B-12.

Dree Andrea
It turns out B-12 is a really big deal. It is one of the essential vitamins affecting various systems of the body. Neurologic, hematologic, gastrointestinal, as well as psychiatric symptoms, arise in cases of deficiency. The reason? Neurotransmitters communicate information throughout the brain and body, relaying signals between neurons. The brain uses neurotransmitters to let your heart know to keep beating, your lungs to inhale and exhale, and your stomach to digest. A lack of B-12 can also affect mood, sleep, concentration, and weight. Vitamin B-12 helps increase brain serotonin and dopamine levels because it is a cofactor in the synthesis of these neurotransmitters, as well as in norepinephrine and gamma-Aminobutyric acid (aka GABA)—the chief inhibitory neurotransmitter in the central nervous system. In humans, GABA also regulates muscle tone.
As I read up on B-12 deficiency, it was like reading my own story: Although not common, psychiatric symptoms may precede the physical ones, including fatigue, forgetfulness, loss of muscle strength, a feeling of pins-and-needles and change in vision. And wouldn’t you know it? The agitation, irritability, negativism, confusion, disorientation, amnesia, impaired concentration and attention and insomnia that a B-12 deficiency can also cause is often misdiagnosed as depression, bipolar or panic disorder, psychosis, phobias, or even dementia.
My doctor administered my first B-12 shot that very day. She warned me that it would take quite some time to start feeling better—up to six months. Me being me, I rushed home to do more research and discovered an alarming number of stories about people who had taken years to recover. A few had to get B- 12 shots for the rest of their lives.
As of December 2017, I had completed my fourth month of replenishing. From onset to diagnosis, almost a year had passed. I am glad to know that I am not going out of my mind.
During those months of self-doubt and uncertainty, a friend convinced me, quite forcefully, to see a therapist who, in turn, referred me to a trauma therapist. Those sessions actually left me questioning whether I would rise out of the ashes ever again. Therapy is not for everyone, and I sensed that this, at least for me, was not the right path. I continued exploring other options to find answers. Looking back, what now seems “crazy” to me is that going down the therapy path might very likely have resulted in a prescription for mood-altering psychotropic medication before my levels of vitamins, minerals, and hormones had been checked out first
And it is dawning on me that B-12 deficiency may be a silent epidemic. According to some studies, four in ten Americans, for example, are not getting enough B-12, while 60 percent of vegetarians and 90 percent (!) of vegans apparently are deficient. A growing number of medical professionals and therapists have also begun talking about a vulnerable third “high-risk” group: highly sensitive people, to which I belong. We perceive emotions, thoughts, and moods, energies, in such an intense way that we are often physically affected or even depleted by other people or situations, or by stimuli such as lights, sounds, or wifi radiation. In my case, adding a B-12 deficiency to an often confusing energy mix could have led to my personal short-circuit. Honestly, I felt I was blowing an emotional fuse. Had I wavered from the belief that I was not mentally ill, I could easily have ended up misdiagnosed with a mental disorder, on lithium or some other antidepressant.
In fact, I looped back to my physician after noticing my mood sink a few days after each B-12 injection—and then rise again while taking the sublingual (under-the tongue) B-12 in between shots. After a little more research, a new gameplan was formulated with the help of an orthomolecular practitioner, which involved no injections and a combination of two different types of sublingual B-12, 3000 mcg methylcobalamine and 3000 mcg adenosylcobalamine. Each one includes folic acid and is held under the tongue for a half-hour for optimal absorption.
Long story short, B-12 deficiency can be a complicated and highly personal journey. And because it is not part of the standard ordered lab work, it requires asking your doctor to test for B-12 if you suspect you have symptoms.
While my viewpoints on health and wellness have not significantly changed, I understand that the mind-body connection is not for everyone. I remain firm in my belief that physical problems arise as a result of something emotionally off-balance in life. During this whole ordeal, I knew that the path back to my old joyous and energetic self would require continuous truthful self-exploration, a combination of the right foods and supplements, and most of all patience. I am still not a huge fan of doctors, but I do recognize the value of a second opinion.
READ THE LABEL

www.istockphoto.com
My blood work revealed a number of vitamin and mineral deficiencies, for which I took various supplements to replenish. It was suggested that I try melatonin to help me sleep. That first night I woke up more often, feeling more severe disorientation and terror than ever before, so I immediately stopped taking it. A few weeks prior to this writing, I suddenly recalled that in my shamanic education we were told to take melatonin in combination with B-6 to enhance practicing lucid dreaming and astral travel. I myself had chosen not to take the supplements at the time. I decided to check the label on the bottle I bought a year ago. Sure enough, on the front in huge letters it said MELATONIN, but in examining the small print I found that the capsules contained a whopping 10 mg of B-6—500% of the daily recommended value!—in addition to the 1 mg of melatonin in each pill. I was shocked to find, returning to the health food store, what other ingredients are added to many vitamin supplements without a clear indication. Turns out we have to start reading those labels as carefully as we read the ones on our food.
 HUNTER GATHERER
HUNTER GATHERER
During my ordeal, a number of my friends brought up the fact that I do not eat meat, which is a good source of B-12. The suggestion I think is that my wounds, on some level, were self-inflicted. It is true that vegans and vegetarians are more likely to be confronted with this problem. Having been a vegan myself for about a year in 2005 during my education as a chef, I respect their choice, even if it means committing to a regimen of B- 12 injections to avoid killing animals. I have opted for eating fish and organic eggs again, thanking the fish and chickens for their offerings. And I have upped my intake of sardines and salmon, which are two of the best B-12 sources, making peace with the fact that I am, like many other animals, a hunter, and gatherer.
 Editor’s Note: Dree Andrea is an international award-winning filmmaker, artist, and energy coach working in New York and New Jersey. Her B-12 journey has taken her in some fascinating directions and led her to some eye-opening studies on B-12 deficiency. There is research that suggests that her hypersensitivity may have been further amplified by the fact that her mother carried twins, but that her sibling died in the womb. She is currently enrolled in the only training that specializes in coaching highly sensitive people and empaths. Dree is working on her second book, The Empath and the Psychopath, and on the documentary Losing Your Marbles; A B-12 Side Effect. Dree can be found at dreeinthebigcity.com.
Editor’s Note: Dree Andrea is an international award-winning filmmaker, artist, and energy coach working in New York and New Jersey. Her B-12 journey has taken her in some fascinating directions and led her to some eye-opening studies on B-12 deficiency. There is research that suggests that her hypersensitivity may have been further amplified by the fact that her mother carried twins, but that her sibling died in the womb. She is currently enrolled in the only training that specializes in coaching highly sensitive people and empaths. Dree is working on her second book, The Empath and the Psychopath, and on the documentary Losing Your Marbles; A B-12 Side Effect. Dree can be found at dreeinthebigcity.com.
A trinity of benefactors advances nursing education.
By Kathryn C. Salamone
Haiti… where natural disasters like the 2010 earthquake and Hurricane Matthew in 2016 exacerbate already unforgiving conditions for its 10 million-plus people who live in abject poverty; where more than half of the population is undernourished and 800,000 people experience food insecurity every day, and where nearly 10,000 people have died of cholera since an outbreak in 2010, the first in a century.
Despite being the poorest country in the Western Hemisphere, despite the existence of an ill-equipped and under-staffed healthcare system—25 physicians and 11 nurses serve 100,000 people—Haiti can now look forward to better health among its people.
Thanks to the combined efforts of the Trinitas School of Nursing (TSON), the College of Saint Elizabeth (CSE), and the Sisters of Charity of Saint Elizabeth (SC), healthcare leaders in New Jersey form a virtual league of healthcare “Avengers.”
 As the program began to take shape, The Haiti Student Nurse Project soon became known as Global Connections in Nursing Education: Haiti and the USA – a name that aptly communicates its essence: assuring that Haitian nurses have access to learning the best practices used in the US that they can then apply in responding to the needs of their fellow Haitians. Since 2014, the program has educated student nurses enrolled at Université de Notre Dame in Jacmel, Haiti, located about 100 miles south of Port au Prince. Its goal: to improve healthcare by strengthening the competence of its nurses. The student nurses have flown to New Jersey to undergo total immersion in US nursing practices and procedures, making the program one of the very few, if not the only one of its kind, to bring students to the United States for their learning experience.
As the program began to take shape, The Haiti Student Nurse Project soon became known as Global Connections in Nursing Education: Haiti and the USA – a name that aptly communicates its essence: assuring that Haitian nurses have access to learning the best practices used in the US that they can then apply in responding to the needs of their fellow Haitians. Since 2014, the program has educated student nurses enrolled at Université de Notre Dame in Jacmel, Haiti, located about 100 miles south of Port au Prince. Its goal: to improve healthcare by strengthening the competence of its nurses. The student nurses have flown to New Jersey to undergo total immersion in US nursing practices and procedures, making the program one of the very few, if not the only one of its kind, to bring students to the United States for their learning experience.
Sister Janet Lehmann, SC, a past chair of the Nursing Program at the College of Saint Elizabeth, envisioned an innovative collaboration with the TSON and CSE. As the current Dean at the Jacmel campus of the Université de Notre Dame, Sister Janet knew that a partnership between the two New Jersey learning institutions could be invaluable to a nation so desperately in need of improved healthcare.
She called TSON and CSE to propose a bold, lasting and beneficial venture. “I asked for faculty and curriculum support plus the opportunity for 12 of my junior nursing students to gain bedside patient care,” Sr. Janet explains. “In Haiti, nursing education relies heavily on memorization which can limit a nurse’s ability to retain the knowledge needed to respond quickly, efficiently. It’s a constant challenge to call to mind what’s needed for competent patient care. From the planning stages, we realized the education program should concentrate on teaching
‘hands-on’ care.”
During the two-week immersion programs in 2014 and again in 2016 at the TSON’s Simulation Lab located in the Elizabeth I. Kellogg Building at the Union County College Elizabeth campus, the student nurses cared for computer-controlled “sim patients.” Sister Janet added, “The student nurses could perform their nursing care in different scenarios with greater confidence as they improved their critical thinking skills.”

Seasoned nursing professionals at TSON and CSE bought into the partnership without hesitation: Mary Beth Kelley, recently retired Dean of TSON, who served more than 40 years in that role, and Professor Eileen Specchio of the CSE Nursing Program who herself has 30 years
behind her.
Dean Kelley notes, “From the beginning, we took great care in developing the in-depth curriculum. Creolespeaking faculty members of TSON translated in both Creole and French and CSE Nursing program graduate students and alumni were heavily involved. Experienced clinical specialists from Trinitas Regional Medical Center and Saint Clare’s Hospital in Denville, another SC sponsored hospital, and those like SC who provided administrative support became a team of ‘super heroes’ who helped bring our vision to reality.”

The program received support from a trinity of benefactors. In addition to the use of the TSON lab, the Trinitas Health Foundation approved a grant that funded the purchase of the simulation equipment specifically designed for countries like Haiti. CSE offered its dorms for the students during their stay.
“We created a challenging environment to educate Haitian nurses so they could gain greater competence and confidence in patient care,” says Dr. Specchio. “Our vision of a global outreach to initiate real change in nursing care in Haiti, our experience with the students, the results we’ve seen in Haiti, all show that we’ve succeeded.”
 FOCAL POINTS
FOCAL POINTS
Global Connections in Nursing Education: Haiti and the USA has lived up to its goal of answering global health needs that the World Health Organization and the International Council of Nurses have identified: to design education programs to promote better health, reduce disease burdens, and lower risk factors.
Here’s what the Trinitas program has concentrated on:
• Hygiene, sanitation/waste control
• Infectious disease, asepsis, and wound care
• Maternal emergencies: hemorrhage, eclampsia, and dystocia
• Women’s health: STD’s, HIV, condom use, self-breast exam, breastfeeding
• Cardiac disease: hypertension, stroke prevention, congestive heart failure
• hydration/dehydration fluid management
• First aid and disaster management: infant, child and adult CPR, choking
• Mental health: communication/active listening, empathy, learned helplessness, domestic violence, parenting principles
• Children issues: malnutrition, assessment, diarrhea prevention and management, and choking
To learn more about the Trinitas School of Nursing, visit:
www.trinitasrmc.org/school_of_nursing.htm
Maureen Chatfield has distinguished herself as one of the state’s most talked about painters. The Hunterdon County resident embraces experiment and change in the creative process, achieving a compelling balance between abstraction and representation in her work. In a 2015 review, Art News described Maureen as a natural colorist, adding that she “fearlessly mines the spectrum, from the gorgeous reds of Matisse to the rich blacks that conjure Franz Kline’s swashbuckling brushwork and Robert Motherwell’s Elegies to the Spanish Republic to the muted, nuanced shades of Richard Diebenkorn.” By applying layer upon layer of color, the story added, she makes paintings of “palpable presence and pleasure.”

Alex 24″x30″ oil on canvas

Bedminster Field 16” x 20”
oil on canvas

Boulder Hill Cabin 8” x 10”
oil on canvas

Flowers in Urn 11” x 14”
oil on canvas

Bedminster 2 16:x20″ oil on canvas

Still Hollow Farm 14” x 18”
oil on canvas

East End 60″x30″ mixed media

Against the Wall 48” x 60” mixed media

Moontide 30″x60″ mixed media
 Maureen Chatfield lives and works just outside the Mountainville section of Tewksbury Township. The structure she uses as her studio housed an apple jack still in the 1780s. She teaches painting at the Hunterdon Art Museum and her work is exhibited at the Rosenberg Gallery on East 66th St. in New York and Cacciola Gallery in Bernardsville, as well as galleries in Greenwich, Nantucket, Atlanta, and Vail. To see more of her work, visit maureenchatfield.com.
Maureen Chatfield lives and works just outside the Mountainville section of Tewksbury Township. The structure she uses as her studio housed an apple jack still in the 1780s. She teaches painting at the Hunterdon Art Museum and her work is exhibited at the Rosenberg Gallery on East 66th St. in New York and Cacciola Gallery in Bernardsville, as well as galleries in Greenwich, Nantucket, Atlanta, and Vail. To see more of her work, visit maureenchatfield.com.

ELIZABETHTOWN GAS REPRESENTATIVES ADDED HOLIDAY HAPPINESS AND JOY TO BROTHER BONAVENTURE RESIDENTS
Thank you to the representatives from Elizabethtown Gas who visited the residents at Brother Bonaventure Long Term Care Facility recently. They personally delivered blankets and holiday cards to every resident, sang holiday songs along with them, and even helped celebrate a birthday! Not only did everyone love the warm and cozy blankets but many new friendships were made!

TAILGATE WITH TRINITAS RAISES OVER $31,000
On Sunday, December 3, 2017 guests gathered at Shacka-maxon Country Club in Scotch Plains to watch the New York Giants take on the Oakland Raiders. NY Giants greats Ottis Anderson, Stephen Baker and Bill Neill delighted Trinitas supporters. While the Giants did not walk away with a win, Trinitas took home a win by raising over $31,000 in net proceeds! Thank you to everyone who supported this year’s Tailgate with Trinitas event; you are the real MVPs! Pictured above is Stephen Baker “The Touchdown Maker” and Lisa Liss, Trinitas Director of Volunteers having fun together.

SAVE THE DATE AND JOIN US FOR TRINITAS HEALTH FOUNDATION’S 2018 ANNUAL GALA
This year the event will be held on Thursday, May 10th at The Venetian in Garfield, New Jersey. Join us for a fun-filled night with
dinner and dancing to music performed by The Infernos. You’ll also have a chance to win some amazing prizes by participating in our raffle drawing, tricky tray, and silent & live auction.
Please join us as we present the Healthcare Foundation of NJ with the Humanitarian Award and Allscripts with the Celebrating Philanthropy Award. Both organizations are very worthy of recognition.
Can’t join us but still want to support Trinitas? Contact the Foundation to learn about the many different sponsorship opportunities available, our online advertisement journal and other ways you can participate by donating items to our tricky tray and silent/live auction.
For more information contact Kim Boyer, Director of Fundraising Events, at (908) 994-8249 or kboyer@trinitas.org.
For more and more summer camps, nutrition is now on the menu.
By Mark Stewart
Of my many vivid summer camp memories, I am struck by how often they revolve around some aspect of food. I was a reluctant eater back then (not anymore) so naturally, I have quite a few culinary-nightmare tales to tell. I was horrified when I discovered that the much-celebrated campfire burgers were cooked on a metal bed frame from the 1930s. The camp spaghetti sauce, which I refused to touch much less eat, looked like it came from Custer’s Last Stand. I also recall being deeply offended that the toast served at breakfast each morning was brown and rock-hard on one side and essentially uncooked on the other. I’m pretty sure it was broiled Wonder Bread.
And yet, lo these many decades later, I am still tempted to purchase a quarter-pound of the cheap bologna at our local grocery store, pair it with a slice of imitation cheese food, and then slather on so much yellow mustard and fake mayo that it oozes out the sides of the sandwich. Ah, memories.
The backstory is that a group of us older campers had set out deep into the Adirondacks on an overnight hike. A three-day storm surprised us and we had to ride it out in a lean-to, with little more than meticulously rationed Gorp to sustain us. I almost strangled a kid over an unclaimed M&M. Anyway, when we dragged our famished 13-year-old bodies back into camp, the cooks were nowhere to be found and all we could scrounge were the aforementioned mystery-meat sandwiches. On my initial bite, the MSG, sodium, and preservatives ignited in my mouth like Sweet Tart fireworks and literally made me shudder. I’m still not sure what cyclamates are, but I’ll bet there were tons of ’em between those flabby slices of white bread.
And curse it all…I don’t think anything has ever tasted that good since.
If I’ve ruined your appetite, I apologize. The good news is that it’s highly improbable that your kids will share anything like this experience when they go off to camp this June or July. Day camps, sleep-away camps, tech camps, sports camps, you name it, have really stepped up their game where nutrition and food quality are concerned. Okay, they still serve burgers and dogs and chicken nuggets. But the meat is no longer the mystery. It’s probably low-fat and preservative-free. In fact, any of those three camp classics may even be meatless. It’s all about providing healthier meal options—a goal that begins with a nutritional philosophy at the top of the camp food chain and trickles down to the cooks and counselors.
 We as parents know that healthy food can be delicious. Fruit and yogurt are smarter breakfast choices than Lucky Charms; salads and whole-grain sandwiches beat Sloppy Joe’s for lunch; and lean grilled meats and vegetables are a vast improvement over high-fat, high-carb, high-sodium dinners like the one the cooks at my old camp titled “turqué alla king.” (I hope at least they used real king, since it was the only part of the dish that was not misspelled.) We can’t always convince our kids to eat right, but it’s encouraging to know that camps now have our backs when it comes to sending the right message.
We as parents know that healthy food can be delicious. Fruit and yogurt are smarter breakfast choices than Lucky Charms; salads and whole-grain sandwiches beat Sloppy Joe’s for lunch; and lean grilled meats and vegetables are a vast improvement over high-fat, high-carb, high-sodium dinners like the one the cooks at my old camp titled “turqué alla king.” (I hope at least they used real king, since it was the only part of the dish that was not misspelled.) We can’t always convince our kids to eat right, but it’s encouraging to know that camps now have our backs when it comes to sending the right message.
As anyone in the camp business will tell you, doing so is in their best interest. It requires a lot of energy to plow through a typical day of activities, and healthy food and snacks are the fuel that makes campers go. You definitely don’t want kids to crash and burn in the middle of a robotics showdown or in the front of a canoe.
 What should campers be consuming? The U.S. Department of Agriculture—the same folks that brought you the much-maligned food pyramid—actually has an answer. The USDA’s MyPlate initiative lays out an ideal, albeit aspirational, set of guidelines for kids to follow. It’s no longer a pyramid. It’s a pie chart and pie is nowhere to be found. It suggests a daily diet of 30 percent grains, 40 percent vegetables, 10 percent fruits, and 20 percent proteins. A smaller circle is dedicated to dairy products, including milk and yogurt. The MyPlate program also preaches portion control. Do summer camps adhere to these guidelines? Some do. The rest are getting there.
What should campers be consuming? The U.S. Department of Agriculture—the same folks that brought you the much-maligned food pyramid—actually has an answer. The USDA’s MyPlate initiative lays out an ideal, albeit aspirational, set of guidelines for kids to follow. It’s no longer a pyramid. It’s a pie chart and pie is nowhere to be found. It suggests a daily diet of 30 percent grains, 40 percent vegetables, 10 percent fruits, and 20 percent proteins. A smaller circle is dedicated to dairy products, including milk and yogurt. The MyPlate program also preaches portion control. Do summer camps adhere to these guidelines? Some do. The rest are getting there.
As a parent, it is probably unreasonable to expect a dietary expert to be looming over the shoulder of each and every camper. But you can ask good questions about a camp’s nutritional philosophy. For example:
- How often does the camp provide sweet snacks and desserts, such as cookies and ice cream? Once a day is okay. More often might be reason for concern.
- What kind of proteins are on the menu? Lean meats, chicken and fish are ideal; the healthier versions of burgers and dogs are fine.
- Are sweet and sugary drinks always available? If so, you know your kid is going to go for those. Low-fat milk and water are preferable, along with some juice in the morning.
- What percentage of bread, rice, cereal and other grains served at camp is whole grain? It’s not difficult or expensive to achieve a 50–50 split.
- What percentage of the food consumed is fruits and/or vegetables? Again, a 50–50 split is an achievable goal.
In many cases, summer camps cover this territory well on their web sites. Food and nutritional information may be listed under a Medical or Wellness tab on the home page. The word you want to look for (or ask about, if it’s not there) is “dietician.” This is a food professional who oversees the content and quality of the camp’s menus and hopefully is involved on some level in educating campers about healthy eating.
A good example of this shift is Campus Kids, a weekday sleep-away camp in Blairstown. Eight years ago, the camp added a staff specialist who oversees the menus and helps manage food allergies, as well as the overall medical needs of campers. Owner/operator Tom Riddleberger acknowledges that more and more children have allergies and food preferences that must be accommodated and managed, but says it’s actually not a big deal.
“This is a trend we are seeing throughout society,” he says, “which in general has become much more open to recognizing individual needs. Food service personnel have moved with the times, and have that expertise. I think the key from a camp perspective is not to have an attitude about accommodating someone’s requests or needs. Homesickness is a need, and camps have always dealt with that. If a child is vegetarian or gluten-free or lactose intolerant, we deal with that smoothly, too, in a way that doesn’t make the child feel singled out.”
I think it’s safe to say that, back in the bologna-sandwich Stone Age days of summer camp, the concept of hiring a staff member with actual nutritional expertise never crossed anyone’s mind. Camp directors were more focused on swimming, boating, hiking, sports, outdoor skills, arts & crafts, and activities and challenges that nourish a young person’s spirit.
Which is where the emphasis still should be.
Indeed, the search for the right-fit summer camp is all about the quality of experience available to your child, about the confidence- and skill-building opportunities offered. Today’s camps are all about nourishing the body and mind, often in ways we could not have imagined a generation ago. Just don’t forget that they’re feeding your kid, too.
 DEALING WITH ALLERGIES
DEALING WITH ALLERGIES
According to the CDC, food allergies among children have increased by more than 50 percent in the last two decades. This has had a huge impact on summer camps, which need to understand who they can and cannot accommodate—and communicate this clearly to parents. In this case, communication is a two-way street. It is incumbent upon parents to be crystal clear with prospective camps about the nature and extent of a child’s allergies, both to food and also environmental allergies.
Another hurdle that summer camps may soon encounter is the possibility that childhood food allergies will fall under the Americans with Disabilities Act. Indeed, there are a great many camps right now that are ADA-compliant but might lose that designation if allergies are classified as a disability.
 PEAK PERFORMANCE
PEAK PERFORMANCE
With the steady rise in the number of sports camps in the country, diet and nutrition have become part of teaching athletes to hone their competitive edge. U.S. Soccer, which oversees the training of the sport’s elite competitors, has issued a set of guidelines for its players, including:
- Choose the least processed foods possible
- Consume lean protein and fruits/vegetables at each meal
- Eat healthy fats (i.e. fish, nuts, avocados)
- Have breakfast within 30 minutes of waking up for max energy
- Make 4 to 6 small meals throughout the day
- Have a high-carb, high-protein recovery meal or shake after workouts
- Stay hydrated at all times
An examination of songs in the key of M.D.
By Luke Sacher
Everyone, at some point in their lives, needs a note from the doctor. So don’t doctors deserve a note or two? During the Rock n Roll age, writing pop tunes about healthcare professionals hasn’t always been a prescription for success, but every so often the result is solid gold. The all-time Top 10 includes songs by legendary groups like the Rolling Stones and Ramones—and individual stars such as Jackson Browne and Robert Palmer—as well as throw-away novelty hits that have managed to stand the test of time. If you’re feeling the end-of-winter blues, here’s my prescription for a little fun…
 ADDICTED TO LOVE
ADDICTED TO LOVE
ROBERT PALMER
Palmer’s signature song won the 1986 Grammy Award for Best Male Rock Vocal Performance and also was nominated for Song of the Year. It entered the Billboard Hot 100 in February 1986, hitting #1 after 13 weeks and was #10 overall for that year. It also hit #1 in Australia and #5 in the UK. “Addicted to Love” was one of the last 45 RPM singles to receive a million-selling Gold certification.
Palmer, who died of a heart attack in 2003 at age 54, said that he wrote the song about his own addictive personality. Originally, he intended it to be a duet with Chaka Khan, but Palmer had to cut the track without her when her record company (Warner Brothers) would not grant her a release to work on his label (Island Records). The anchoring guitar chords for the song came to him in a dream: “That noisy riff woke me up. I went downstairs, got out the tape recorder, then went back to bed. Next morning, I thought, Phew, caught one there!”
The iconic music video for the song, directed by British photographer Terence Donovan, featured Palmer performing with a “band” of top female fashion models. Their visual style—pale skin, heavy makeup, dark hair, and seductively detached expressions—was derived from the paintings of Southern California pop artist Patrick Nagel. They were cast precisely because they had no musical training. As a result, each was keeping her own time and moving to a different beat. Palmer and Donovan reprised the visual concept for his videos for three other songs, including “Simply Irresistible.”
 COMFORTABLY NUMB (THE DOCTOR)
COMFORTABLY NUMB (THE DOCTOR)
PINK FLOYD
First released on the band’s 1979 album The Wall, “Comfortably Numb” was one of only three songs on the album co-written by guitarist David Gilmour and bassist Roger Waters. They were at loggerheads while working on it. “We argued over ‘Comfortably Numb’ like mad,” Gilmour later said. “Really had a big fight, went on for ages.”
They finally agreed to use Waters’s preferred opening and Gilmour’s second solo in the final mix. The lyrics are a counterpoint between the remarks of a doctor treating embittered rock star Pink (verses sung by Waters) and Pink’s inner monologue (chorus sung by Gilmour). The inspiration for Waters’s lyrics stemmed from a personal experience during the band’s 1977 In the Flesh tour: “I had stomach cramps so bad that I thought I wasn’t able to go on. A doctor backstage gave me a shot of something that I swear to God would have killed…an elephant. I did the whole show hardly able to raise my hand above my knee…That was the longest two hours of my life.”
When the band came out for an encore, Waters was unable to join them.
“Comfortably Numb” was ranked #5 on BBC Radio’s Desert Island Discs list and is lauded for its two virtuoso guitar solos. It also claims the distinction of having been the last song ever to be performed together by the original band members (Roger Waters, David Gilmour, Richard Wright and Nick Mason), in 2005.
 DOCTOR MY EYES
DOCTOR MY EYES
JACKSON BROWNE
“Doctor My Eyes” was the first single from Browne’s 1972 debut album and was a surprise hit for Geffen Records, reaching #8 on the Billboard Hot 100. The lyrics are essentially the reflections of a young man explaining to his psychotherapist how he had managed to endure the slings and arrows of life by steeling himself with stoicism—only to discover that it had rendered him isolated, emotionally bereft, and despondent. At the suggestion of David Geffen, Browne reworked what was composed as a slow ballad by upping the tempo, adding conga drums, background vocals and a catchy guitar solo—and turning the lyrics’ message of suicidal despair into resigned acceptance.
Browne’s good friends David Crosby and Graham Nash sang harmony vocals. Geffen asked Nash if he thought there was a single on the album, and Nash picked this one, while also recommending that Browne write a high vocal harmony into the chorus. There was originally a third verse to the song, which can be found on rare bootlegs
of the original demo recording. The late Glenn Frey of The Eagles said that he learned how to write songs when he and Browne were neighbors in Echo Park, by listening to him working on the opening piano riff over and over until he got it exactly right. Frey said to him, “So that’s how you do it. Elbow grease.”
 DR. ROBERT
DR. ROBERT
THE BEATLES
Everyone knows today that The Beatles experimented with drugs and wrote songs about their experiences under their influence, including “Lucy in the Sky with Diamonds” and “Magical Mystery Tour.” Was their very first “Dr. Robert,” which was written in 1966 and released in the U.S. on their Yesterday and Today album? In Paul McCartney’s book Many Years From Now, coauthor Barry Miles revealed that the name was based on Dr. Robert Freymann, whose East 78th Street clinic was “conveniently located for Jackie Kennedy and other wealthy Upper East Siders from Fifth Avenue and Park to stroll over for their vitamin B-12 shots, which also happened to contain a massive dose of amphetamine. Dr. Robert’s reputation spread, and it was not long before visiting Americans told John and Paul about him.”
I was six years old in 1966. Growing up on East 81st Street in Manhattan, I thought that it was a song about my Park Avenue pediatrician. I’m pretty certain that my parents knew exactly who Dr. Robert actually was, since he lived only three blocks away. Robert Freymann practiced in New York for almost two decades, administering massive doses of legal amphetamines to silk-stocking district and celebrity clients. He was finally expelled from the New York State Medical Society in 1975 for malpractice.
“We’d hear people say, ‘You can get anything off him, any pills you want,’” McCartney said. “It was a big racket. The song was a joke about this fellow who cured everyone of everything with all these pills and tranquilizers. He just kept New York high. John and I thought it was a funny idea: the fantasy doctor who would fix you up by giving you drugs, it was a parody on that idea.”
 I DON’T NEED NO DOCTOR
I DON’T NEED NO DOCTOR
NICK ASHFORD, VALERIE SIMPSON, JO ARMSTEAD
Written by the legendary Motown husband-and-wife songwriting and performing team of Ashford & Simpson —in partnership with the equally marvelous “Joshie” Armstead—“I Don’t Need No Doctor” is considered one of the quintessential R&B tunes of the 1960s. It actually draws on elements of Gospel, Soul and Rock, which, over the years, has made it one of the most-recorded “doctor songs” in history.
Ashford & Simpson penned iconic hits including “Ain’t no Mountain High Enough” and “Ain’t Nothing Like the Real Thing,” while Armstead started her career as creator and lead singer of Ike and Tina Turner’s Ikettes, in 1961. “I Don’t Need No Doctor” was first recorded by Ray Charles and his orchestra in 1966. The 1971 version by Humble Pie still gets plenty of requests on oldies stations.
The tune has been covered by artists of all genres, from heavy metal to jazz, including: The Chocolate Watchband (1969), The New Riders of The Purple Sage (1972), W.A.S.P. (1986), Great White (1987), The Nomads (1989), Roseanna Vitro (1997), Beth Hart (2004), Styx (2005), Dr. Sin (2005), John Scofield (2005), John Mayer (2007), Joan Osborne (2012), Secret Affair (2012), Demented Scumcats (2014), The Sonics (2015), and the Lost In Paris Blues Band (2016), featuring guitarist Robben Ford
 I WANNA BE SEDATED
I WANNA BE SEDATED
THE RAMONES
One of the band’s best-known songs, it was originally released on their fourth album, Road to Ruin, in September 1978. Joey Ramone came up with the idea for the song after he burned himself severely with boiling water and was rushed to a hospital. (He regularly inhaled steam from a kettle before concerts to help clear his nasal passages.) The chorus lyrics Nothing to do, nowhere to go—oh oh were inspired by The Ramones’ tour stop in London, which they discovered completely shut down at Christmas time.
“There’s nothing to do, nowhere to go,” Joey recalled. “Here we were in London for the first time in our lives, and me and Dee Dee were sharing a room in the hotel, and we were watching The Guns of Navarone on TV. I mean, here we are in London finally, and this is what we are doing, watching American movies in the hotel room.”
Johnny Ramone played the same note 65 times in a row in his guitar solo. (How “punk” can you get?). It’s the recording on which Marky Ramone performed as the band’s drummer after replacing Tommy Ramone, who began producing their records. Marky said that it was completed very quickly in the studio, and that his part took only two takes. Ten years after the song was released, Director Bill Fishman made an iconic video for it: one continuous master shot of the Ramones sitting at a kitchen table nonchalantly reading and eating corn flakes while hyperkinetic nuns, acrobats, ballerinas, monsters, cheerleaders, clowns, naughty nurses, and schoolgirls (including a very young Courtney Love) run around them and try to grab their attention.
 LIKE A SURGEON
LIKE A SURGEON
“WEIRD AL” YANKOVIC
Of all the things that songwriters write about, surgery has to be one of the least popular. After a thorough search through cyberspace, this parody of Madonna’s “Like a Virgin” was literally the only hit song I could find. Recorded in 1985 by Weird Al Yankovic for his third studio album, Dare to Be Stupid, it was written by Yankovic and Madonna herself (who came up with the title), while guitarist Rick Derringer was its executive producer. Prior to this recording Weird Al had never used ideas from other musicians. A mutual acquaintance of both his manager and Madonna’s suggested that they would have good fun collaborating on it. It’s the only known time that he ever worked on one of his parodies directly with the original artist.
“Like a Surgeon” was well received by music critics. Many rated it on par with the original. Eugene Chadbourne congratulated Yankovic for “…perhaps his best ever. Turning the tacky Madonna hit inside out and upside down, he comes up with a hilarious satire of the medical profession.” The music video produced for the tune is set in a hospital, and vamps on elements of the original music video for “Like a Virgin.” In one scene, a Madonna lookalike sits in a corner, filing her nails. It has been a part of Yankovic’s live shows for decades.
 MOTHER’S LITTLE HELPER
MOTHER’S LITTLE HELPER
THE ROLLING STONES
Valium (aka diazepam) is a synthetic analog to the active ingredient found in Valerian root; both increase the amount of a chemical called gamma aminobutyric acid (GABA) in the brain, which helps regulate nerve cells, and has a calming effect on anxiety. “Mother’s Little Helper” is both an ode to this drug…
Mother needs something today to calm her down.
And though she’s not really ill,
There’s a little yellow pill.
She goes running for the shelter
Of a Mother’s Little Helper.
…and a biting commentary on the hypocrisy of American housewives abusing prescription drugs with the benediction of their doctors and the FDA, while the Stones themselves were being labeled dope fiends, simply for taking different drugs without a prescription. Both were seeking refuge from emptiness and despair. Recorded in Los Angeles from December 3 to 8, 1965, in a custom built studio with no windows (the Stones did not want to know if it was day or night), it was the first track on Aftermath, their first album with all original songs.
“It’s about drug dependence, but in a sort of like spoofy way,” Mick Jagger observed.
About his strange-sounding guitar work, Keith Richards said he used a twelve-string with a slide on it: “It’s played slightly Oriental-ish. The track just needed something to make it twang. Otherwise, the song was quite Vaudeville, in a way. I wanted to add some nice bite to it. And it was just one of those things where someone walked in and, ‘Look, it’s an electric twelve-string’. It was some gashed-up job. No name on it. God knows where it came from—or where it went. But I put it together with a bottleneck. Then we had a riff that tied the whole thing together.”
Stones guitarist Brian Jones played the Sitar on the recording. It was one of the first pop songs to use the instrument, just after The Beatles’ “Norwegian Wood.” Drummer Charlie Watts says the band never quite mastered playing it live, although they memorably performed it on The Ed Sullivan Show.
 THEY’RE COMING TO TAKE ME AWAY
THEY’RE COMING TO TAKE ME AWAY
(FUNNY FARM)
NAPOLEON XIV
Music critic Dave Marsh called “Funny Farm” the most obnoxious song ever to appear on a jukebox. In 1966, Jerry Samuels (alias Napoleon XIV) was a top recording engineer at New York City’s Associated Recording Studios in Times Square. One night he and Barry Hansen (alias Dr. Demento) were “relaxing” when an old Scottish march called “The Campbells Are Coming” popped into his head.
“I thought, da da dat dat da dat, da da, da da. They’re coming to take me away, ha ha… We were doing work for some advertising agencies, radio spots. They had to come in at exactly 59 seconds, so if it was recorded a little slow or a little fast, we used a device to fix it called a Variable Frequency Oscillator. We only had a 4-track tape recorder at the time. But if you hooked up the VFO to the 4-track, you could do things that weren’t done before. I would be able to raise or lower the pitch of a voice without changing the tempo. By understanding what I could do with that piece of equipment, I wrote this thing.”
Samuels was hesitant to complete the song, which was a sick joke about a serious subject, mental illness. After many months he changed the last verse to say “They’re coming to take me away” because of his dog running away. “By doing that I felt I was lightening the sickness of the joke.”
Adding to the overall silliness, the B-side of the 45 rpm single was simply the A-side run in reverse, and titled “!aaaH-aH ,yawA eM ekaT oT gnimoC er’yehT” (Ha-Haaa! Away, Me Take to Coming They’re). The song was an overnight sensation, peaking at #3 on the Billboard Hot 100, but plummeted to #37 only two weeks later. Fearing outrage from those who thought that it was ridiculing mental illness, radio stations across the country— including New York City’s WABC and WMCA—banned it from their playlists. Airplanes flew protest banners and mobs of angry teenagers picketed WMCA, holding signs saying We’re Coming to Take WMCA Away.
 WITCH DOCTOR
WITCH DOCTOR
ROSS BAGDASARIAN
(aka DAVID SEVILLE)
Ross Bagdasarian (David Seville) was a successful songwriter by the time he released “Witch Doctor” as his first single. Seven years earlier, he’d written “Come On-A My House,” one of Rosemary Clooney’s signature hits. The lyrics were based on lines from the novel The Human Comedy, written by his famous cousin, William Saroyan. Bagdasarian was the creator of Alvin and The Chipmunks, a group of three animated rodents with high-pitched human voices. He created the effect by recording his voice with a tape recorder running at half speed, then playing it back at normal speed. “Witch Doctor” was the first song ever to use this technique, and he used the name David Seville for the recording. At that point, he hadn’t yet created The Chipmunks. The song is about a young man seeking advice from a witch doctor on how to woo his girlfriend. The wise witch doctor offers him some magic words that, six decades on, way to many of us still know by heart: Oo ee, oo ah ah, ting tang, walla walla bing bang.
“Witch Doctor” soared to #1 in April 1958 for three weeks. Seville became a pop culture sensation, and performed the song on The Ed Sullivan Show that May. It was also a #1 R&B hit. Many R&B art-toppers of the day were comedic or novelty recordings, including “Get a Job” by The Silhouettes and “Yakety-Yak” by The Coasters. A few months later, using the same technique, Seville created and recorded three distinct voices in close harmony and branded it “The Chipmunks.” In November, he released “The Chipmunk Song (Christmas Don’t Be Late),” which went to #1 for four weeks, won three Grammy Awards, and became a perennial Christmas favorite. The Alvin Show cartoon series followed in 1961—and was resurrected in 1983, and again in 2015.
Album Art: Addicted to Love/Island Records • Comfortably Numb/Columbia Records • Doctor My Eyes/Asylum Records • Dr. Robert/Capitol Records • I Don’t Need No Doctor/A&M Records • I Wanna Be Sedated/Sire Records • Like A Surgeon/Scotti Brothers • Mother’s Little Helper/London Records • Funny Farm/Warner Bros. • Witch Doctor/Liberty Records
EDGE takes you inside the area’s most creative kitchens.
 Paragon Tap & Table • Beef Ramen
Paragon Tap & Table • Beef Ramen
77 Central Ave. • CLARK
(732) 931-1776 • paragonnj.com
As we constantly introduce new flavors from around the world to our customers at Paragon Tap and Table we have added an Asian inspired Noodle Dish with a touch of the south. Our beef ramen noodle showcases all the characteristics of a traditional ramen but twisted with the smokiness of the smoked beef brisket.
— Eric B. LeVine, Chef/Partner
 Arirang Hibachi Steakhouse • Wasabi Crusted Filet Mignon
Arirang Hibachi Steakhouse • Wasabi Crusted Filet Mignon
1230 Route 22 West • MOUNTAINSIDE
(908) 518-9733 • partyonthegrill.com
We prepare a crusted 8-ounce filet mignon served with gingered spinach, shitake mushrooms, and a tempura onion ring.
 Daimatsu • Sushi Pizza
Daimatsu • Sushi Pizza
860 Mountain Ave. • MOUNTAINSIDE
(908) 233-7888 • daimatsusushibar.com
This original dish has been our signature appetizer for over 20 years. Crispy seasoned sushi rice topped with homemade spicy mayo, marinated tuna, finely chopped onion, scallion, masago caviar, and ginger. Our customers always come back wanting more.
— Chef Momo
 The Barge • Cioppino
The Barge • Cioppino
201 Front Street • PERTH AMBOY
(732) 442-3000 • thebarge.com
Our Cioppino, the signature dish of San Francisco, features a fresh, healthy selection of clams, mussels, shrimp, Maine lobster and Jersey scallops—drizzled in Greek virgin olive oil, with fresh garlic and white wine—over homemade Italian linguini. I know it will become one of your favorite dishes
 Luciano’s Ristorante & Lounge • Jumbo Lump Crab Cake Bruschetta
Luciano’s Ristorante & Lounge • Jumbo Lump Crab Cake Bruschetta
1579 Main Street • RAHWAY
(732) 815-1200 • lucianosristorante.com
Jumbo lump crab cake bruschetta, finished with virgin olive oil and a balsamic reduction has been one of Luciano’s signature appetizers since we opened.
— Joseph Mastrella, Executive Chef/Partner
 Morris Tap & Grill • The Monster Burger
Morris Tap & Grill • The Monster Burger
500 Route 10 West • RANDOLPH
(973) 891-1776 • morristapandgrill.com
As the leader in the gastropub world in New Jersey, Morris Tap and grill has been providing creative, quality, fresh certified burgers for over 6 years. Here’s an example of what we do creatively with our burgers, The Monster Burger. Two certified angus beef burgers topped with chorizo sausage, slaw, bacon, cheddar cheese and a fried egg!
— Eric B LeVine, Chef/Partner
 LongHorn Steakhouse • Outlaw Ribeye
LongHorn Steakhouse • Outlaw Ribeye
272 Route 22 West • SPRINGFIELD
(973) 315-2049 • longhornsteakhouse.com
LongHorn Steakhouse has opened in Springfield, and we are looking forward to meeting all of our future guests! When you visit us, we suggest you try our fresh, never frozen, 18 oz. bone-in Outlaw Ribeye—featuring juicy marbling that is perfectly seasoned and fire-grilled by our expert Grill Masters.
— Anthony Levy, Managing Partner
 Outback Steakhouse • Bone-In Natural Cut Ribeye
Outback Steakhouse • Bone-In Natural Cut Ribeye
901 Mountain Avenue • SPRINGFIELD
(973) 467-9095 • outback.com/locations/nj/springfield
This is the entire staff’s favorite, guests rave about. Bone-in and extra marbled for maximum tenderness, juicy and savory. Seasoned and wood-fired grilled over oak.
— Duff Regan, Managing Partner
 Arirang Hibachi Steakhouse • Volcano Roll
Arirang Hibachi Steakhouse • Volcano Roll
23A Nelson Avenue • STATEN ISLAND, NY
(718) 966-9600 • partyonthegrill.com
Hot-out-of-the-oven, crab, avocado and cream cheese rolled up and topped with a mild spicy scallop salad.
 Galloping Hill Caterers
Galloping Hill Caterers
Galloping Hill Road and Chestnut Street • UNION
(908) 686-2683 • gallopinghillcaterers.com
Galloping Hill Caterers has been an incredible landmark for nearly sixty years. We pride ourselves in delivering “over the top” cuisine, impeccable service and outstanding attention to detail. That is the hallmark of our success! Simply, an unforgettable experience. Pictured here is one of our crepes flambé that really creates lots of excitement!
— George Thomas, Owner
 Ursino Steakhouse & Tavern • House Carved 16oz New York Strip Steak
Ursino Steakhouse & Tavern • House Carved 16oz New York Strip Steak
1075 Morris Avenue • UNION
(908) 977-9699 • ursinosteakhouse.com
Be it a sizzling filet in the steakhouse or our signature burger in the tavern upstairs, Ursino is sure to please the most selective palates. Our carefully composed menus feature fresh, seasonal ingredients and reflect the passion we put into each and every meal we serve.
 Vine Ripe Markets • Filet Crostini with Horseradish Cream Sauce
Vine Ripe Markets • Filet Crostini with Horseradish Cream Sauce
430 North Avenue East • WESTFIELD
(908) 233-2424 • vineripemarkets.com
Savory, tender, with a touch of aromatic and toasted flavors that tantalize the senses! Filet Mignon served rare and shaved onto homemade Garlic Crostini, topped with our Horseradish Cream Sauce is a medley of tender and crispy textures perfect for sharing with family and friends, any time of year!
— Frank Bruno, Chief Culinary Officer
…you ask your phlebotomist if he got
the whole phleb.
 …you use DNA, DNR and DMV interchangeably.
…you use DNA, DNR and DMV interchangeably.
…when your doctor asks you to “Fill this cup for me”
you can’t resist asking “From here?”
…when the same doctor finishes your colonoscopy she says,
“Bad news. I think you’re head’s still up there.”
 …you have to spell-check MRI.
…you have to spell-check MRI.
…there is no part of your body
you wouldn’t use to stop an elevator from closing.
…instead of doing chest compressions to
the beat of Stayin’ Alive, you do them
to Another One Bites the Dust.

…you stifle a laugh whenever someone says “dopamine.”
 …your advice to someone who broke their leg in
…your advice to someone who broke their leg in
three places is Wow, make sure not to go
back to those places.
…you named your dog MCAT.
…you consider Cyrus Virus
a pre-existing condition.
…“fecal-oral spread” makes you think of hors d’ouevres.
…after all these years, no one has ever laughed
when you tell someone they’re a “sight for
psoriasis.”
 …you think Pepcid AC is a
…you think Pepcid AC is a
South American soccer team.
…it can’t be important if it’s not on the midterm.
…“clinicals” sounds like something you’d scrape off a clinic.
News, views, and insights on maintaining a healthy edge.
 A New Line in the Sand
A New Line in the Sand
Is it possible to develop high blood pressure without seeing your blood pressure rise? The answer is yes. A team of experts assembled by the American College of Cardiology and the American Heart Association has concluded that the new cutoff should be 130-over-80. That immediately puts more than 30 million people in the U.S. into high blood pressure category. The most-affected group is men under the age of 45; the number of men who are “over the line” now triples. The good news is that the new cutoff does not mean that these folks will have to go on medication. The 130-over-80 number will more accurately identify individuals who are at a higher risk for stroke and heart attack—and hopefully a wake-up call to smokers and people who don’t get regular exercise.
 Danger Alert for TV Binge Watchers
Danger Alert for TV Binge Watchers
Doctors have been telling us for years to “get up off the couch” and exercise. Now they are telling us that this won’t do much good if we simply return to the couch. A study conducted by the University of Vermont on the TV-watching habits of more than 15,000 people has found those who say they watch “very often” are 1.7 times more likely to develop dangerous deep-vein blood clots. That in and of itself is hardly surprising. The eye-opening part of the study concerned middle-aged subjects; heavy TV-watchers in that age range who also got 150 minutes of exercise a week appear to have a slightly higher risk of DVT. Bad news for binge-watchers. Bad news for Netflix!
 Now Hear This
Now Hear This
Surgically implanted hearing aids have had a spotty history. Often they fail for the simplest reason: the middle ear is not a one-size-fits-all environment. At a December meeting of the Radiological Society of North America, researchers presented an exciting breakthrough that combines CT scans with 3D printing to produce custom-design implants for the middle ear, where three tiny bones (ossicles) transmit vibrations from the eardrum to the cochlea. Damaged ossicles are reconstructed with prostheses made of stainless steel and ceramics, which have a high failure rate. Dr. Jeffrey Hirsch, who authored the study, points out that the odds of getting a perfect fit are less than 1 in 1,000. In its first trial run, the CT+3D method had spectacular results. “This study highlights the core strength of 3D printing,” says Hirsch of the ability to very accurately reproduce anatomic relationships in space to a sub-millimeter level. “With these models, it’s almost a snap fit.”
 Is Chocolate a “SAD” Solution?
Is Chocolate a “SAD” Solution?
As spring creeps ever closer, the light is at the end of the tunnel for those who suffer from Seasonal Affective Disorder, aka SAD. To make it through these last few weeks, science offers some tools to keep up your spirits. Helping others can be a surprisingly uplifting experience, even if it’s not something you usually do. While volunteerism is at its peak around the holidays, by February and March there is a need for help at local shelters, food pantries, etc. Another option is 30 to 60 minutes of strenuous exercise, such as fast walking or aerobics. Exercising outdoors, even in cold weather, can boost your focus and reduce stress. New research also suggests that exercising under bright lights will have similar benefits. Even when not exercising, exposing yourself to bright light (such as a light box) for a half-hour a day has been shown to be effective for some people as anti-depressants. Here’s the best news: eat high-quality chocolate. It’s a proven mood booster and can relieve anxiety. We’re not talking about candy bars here—they may give you a quick pop, but may also contribute to negative feelings as you come back down.
 Double Trouble
Double Trouble
One of the many ways social media has changed our lives is through the spread of information on alternative cancer therapies. But has it changed our lives for the better? According to a study published in the Journal of the National Cancer Institute, people who choose alternative treatments for commonly curable cancers may double their risk of death. The authors defined “alternative” as a medical treatment administered by a non-medical person. Conventional therapies include chemo, radiation, and surgery. Patients who pursue non-medical options run the risk of allowing their cancers to spread to other parts of the body, including the lymph nodes. The study offers the example of stage-one breast cancer. With traditional treatment, a patient’s five-year survival rate is almost 100 percent. If that cancer is allowed to reach stage four, that survival rate is reduced to 25 percent. The study covered the most common cancers and looked at outcomes of 280 patients who chose alternative medicine versus the outcomes of 560 patients who went the traditional route.
 Is That Cigarette Really Worth Seven Years?
Is That Cigarette Really Worth Seven Years?
Whether we admit it or not, we all keep score as we age. We weigh our bad habits against our good ones and temper those estimates with what we know about our genetics. It’s an inexact science, to be sure…yet not as much as it used to be. University of Edinburgh researchers looked at the genetic makeup of 600,000 individuals from three different continents, zeroing in on genes related to lifestyle choices, including smoking, drinking, overeating and substance abuse. They were able to come up with a fascinating scoring system. For instance, people live an average of two months less for every kilogram they are overweight. Pack-a-day smokers shave off an average of seven years. The study also found that people live an average of 11 months longer for every year of schooling they have. Genes related to cholesterol levels and the immune system also appear to have a dramatic impact on life expectancy. The conclusion drawn by the researchers was that genes play a major role in determining life expectancy, but our lifestyle choices have a far greater impact than most people imagine.
TV Doctor Benjamin Hollingsworth of “Code Black”
What kind of research is involved in playing the role of Dr. Mario Savetti? It takes a lot of hard work and preparation to get to a point where you can convincingly play a doctor on TV. We pride ourselves in our ability to portray the medical world as authentically as possible. I’ve probably done about 300 hours of medical training and boot camp. I understand how to work with a central line, intubation, chest tube, thoracotomy and just about every major ER procedure from start to finish. And I’ve actually gotten good at stitching. When people need their pants hemmed, I can suture to help save on tailoring costs!
In what ways is your personal reality similar to your Code Black character’s?
I live my excitement at work—which is something I think we share—and I also have a competitive nature…but, of course, I don’t save lives. Something else he and I share is that we don’t come from a super-wealthy family. I attended a prestigious acting school, but I had to work my way to get there with barely any connections, and I’ve had to fight for my roles—and I’ve had to really put in the work to get them.
What do you admire about him?
He has this ability to survive. Angels Memorial is one of the toughest places in the world to work, and he not only survives but he excels. I really admire his ability to handle just about every situation thrown at him. He’s very instinctual, which is what makes him such a good ER doctor. He doesn’t question himself. He works really hard to know what he needs to do and he’s good at doing it. That absence of self-doubt is one of his greatest strengths. You co-star in the upcoming action film Hard Powder with Liam Neeson, Laura Dern, Emmy Rossum and William Forsythe.
How does being part of a cast like that help you refine your craft?
Any time you get to share the screen with such talented veterans, you learn. I have conservatory training. I spent three years learning a craft, but one of the biggest things I learned in theater school was that you never stop learning. So even now, a decade after graduating, I’m still going to work and learning from the best.
You did an episode of Degrassi about 10 years ago. Is that some sort of right of passage for Canadian actors?
Yes [laughs] this was my first role out of theater school. It’s definitely a Canadian rite of passage! Degrassi opened up a lot of opportunities. I made a lot of good friends and we stayed in touch. When I first got started down in L.A., they were also there and we would all get together. There were a lot of friendships that formed from the show. It was great.
Editor’s Note: Editor-at-Large Ashleigh Owens actually spent a good 10 minutes with Ben Hollingsworth. To read 5 More Minutes with the Code Black star—and learn about his 2018 film projects— log onto Edgemagonline.com.
You don’t often hear it discussed, but the role of “television nurse” is among the most coveted in the entertainment business. Like real-life nursing, it offers the challenge of creating order from chaos, as well as the opportunity to leave an indelible imprint on every shift. It has supercharged the careers of many of our finest actors (Julianna Marguilies , Maura Tierney, Loretta Swit, and Edie Falco, to name a few) and given us countless unforgettable TV moments. Marlyne Barrett brings something extra-special to the role of Maggie Lockwood, Head Charge Nurse at Gaffney Medical Center in the NBC series Chicago Med. She has a real-life nursing degree, and several family members—including her mother and sister—are medical professionals. While playing a nurse is literally second nature to Barrett, she has been winning critical acclaim for her stage and screen performances for more than a decade, including an unforgettable turn as a crooked politician on The Wire. EDGE editor Mark Stewart wanted to know what it takes to balance the subtle strength and intense conflict her characters exude. As he discovered, it comes naturally. But never easily.
EDGE: I think about the characters you’ve played throughout your career and they are without exception powerful and highly competent women. Do you look for those roles as an actor, or do they find you?
MB: That’s a chicken and egg question, isn’t it? Where you are in your career often mirrors where you are with your characters. What you can play in a rich, dimensional way often determines the roles available to you. What you ask yourself as an actor is: Am I ready to do this role…and is this role ready for me?
EDGE: What are the demands of the Maggie Lockwood character on Chicago Med?
MB: Maggie plays the spirit of the E.D. She’s the one that maintains the professionalism and the humanity. The current of her presence impacts the entire atmosphere. When you initially get a role like Maggie, you’re like I can do it I can do it and you find the swagger in the character, and you’re really excited to have the swagger. Now three seasons in, Maggie is in a place where she’s asking herself about her signature in nursing.
EDGE: It’s interesting how much depth has been added to this character this season. Why now?
MB: I think Maggie is one of those characters that the writers put in their back pocket for later development. You watch these shows where they may introduce new characters in the third season to bring a fresh breath to a show. Chicago Med is a little different. What we’ve decided to do is to develop Maggie slowly, to be kind of an ace in the hole. So you sprinkle her everywhere in seasons one and two, and here we are in the third season expanding Maggie in some really interesting ways.
EDGE: I hope you take a little credit for that.
MB: Oh, definitely. And I’ve enjoyed this process. When you know you’re going to play a character for many years, you want a slow burn. Unless you’re going to do it the British way, where in one season you may have six episodes. As an actor, it’s better to have these back pocket moments with the characters you’re developing.
EDGE: Normally, an actor spends weeks shadowing the real-life version of the person they are playing. Since you had a nursing degree, did you get a reprieve from that? A note from the doctor?
MB: No [laughs] but it was helpful. The cast actually works with Dr. Andrew Dennis frequently for medical rehearsals, but we don’t see nurses that often. However, there was a nurse at Rush University Medical Center in Chicago who influenced how I play Maggie Lockwood. Her name is Gloria. I remember walking into a situation where a woman who had been hit by a semi was wheeled into the emergency room. Her body was pretty damaged. Gloria was so focused, working her environment like a symphony conductor…she had syringes, she was advising nurses what to do, she was assessing the situation, she was not overwhelmed by the urgency. The maturity in her eyes told me she knew exactly what she was doing, And the wrinkles in her face made me understand that there had been a price paid for her talent in nursing.
EDGE: Are those wrinkles familiar?
MB: I definitely recognize them in my sister, who is a doctor, a young doctor. And I recognize them in my mother, who is about to retire as a NICU nurse. The vocation anchors itself in you. It drives a depth of commitment inside you. The deeper you go into this commitment of bringing healing to people’s lives, the more it invades your life. Nursing isn’t just something my mother did. It was part of her language, part of her swagger, part of her education, part of everything. Same thing with my sister.
EDGE: Maggie can be pretty tough on the young doctors and nurses. Did you get pointers from your mother and sister?
MB: I’ve never seen my mother interact with the residents. But it is something I actually witnessed firsthand in nursing school. And I’ve seen it in my sister. Often senior nurses and doctors collaborate to ensure that young doctors become the doctors the profession should have, so being tough is a calculation made to improve and maintain the healing atmosphere you offer patients.
EDGE: If you never planned to work as a nurse, why get the degree?
MB: It was a promise I made to my parents. My father worked for Siemens as a medical engineer. And we have cousins who are doctors and nurses. So it’s a family thing. When immigrants—my family is from Haiti—come into this country, this is what they call “royal” blue-collar jobs. Doctors, nurses, engineers. There is a regal-ness to doing these professions. You can use these jobs to enter any area of society.

Courtesy of NBC Universal
EDGE: Tell me about the friendship you built with Ian McShane (above) while you were on the NBC series Kings.
MB: Everyone, in a number of professions, across the board, says the same thing about that man: Ian McShane is an authentic, incredible human being and a phenomenal artist. Ian was involved in the resurrection of my career. There is a five-year gap in my résumé. I was the victim of an assault. I’m a person who loves to laugh. I love life. I love human beings. After I was assaulted, to say that I was distraught would be an understatement. I became introverted and depressed. I needed a lot of prayer and a lot of counseling, in addition to the physical help I received. During that time of major pain, that’s when I met my husband. I met him a month after the event. He took the time to love on me well. And it was Ian McShane who was my true north.
EDGE: How so?
MB: Ian was there to help me get back on my feet. I thought I was leaving acting for good. He did not think that I was, and he said that when I was ready to come back, I should contact him. When the time came, I reached out to a lot of friends who were A-listers, people with whom I had worked. They said Yeah, I’ll help you. But I never heard from them, really. I made one call to Ian and he had representation ready to hear from me, he had a meeting set up for me, and within two weeks I was back on-air, on American Crime.
EDGE: He has a reputation for being generous as an actor, too.
MB: Yes exactly. You know, I did a scene with Ian on Kings and, after it was done, I was so bummed. I felt like, Man I wish I’d done that a different way. I went to see him the following day and said, “Hey remember that scene we did by the water?” He said, “Ya, doll. It was great, love.” I told him I felt there was something missing there. He said, “No, no. It was great.” I got very serious and told him he had a chance to pass on his gift and make me a part of his legacy. He laughed. And then he gave me the instruction. Well, you could do this, this, this and this— giving me pointers on how he’d approach it. From then on he really expanded my craft. And after Kings, I wanted to do some studying in London. He wrote me a great letter of recommendation to his alma mater, RADA [the Royal Academy of Dramatic Art] and I went on to study there.
EDGE: I would be remiss if we didn’t talk about your two seasons on The Wire. Nerese Campbell (facing page) was a brilliantly conceived character—a politician who used people and power in the same ways the criminals did. You were disturbingly convincing.

HBO/Blown Deadline Productions
MB: Thank you! I made the conscious decision that if Nerese—as a politician—was going to rub shoulders with the boys, we were going to dance. It was Baltimore. And the truth is that I wanted her to go all the way to Washington. I calculated this idea that having a law degree and going into politics, she knew she would be dealing with people who weren’t necessarily refined. So what would I bring to the table when I wanted to sway a situation? I needed something as strong as a gun—something in her speech that was as potent as gunpowder, something so specific that my words balanced between intelligence, wisdom, and a threat. That’s what I thought Nerese was—all in a sexy body. There was one scene that captured her perfectly. She is going to work in her Mercedes on a sunny day, Bubbles is passing by and hands her a newspaper. Her window goes up, she opens the newspaper and we see that her illegal activity is on the front page. She’s exposed. And we see her, through the window, cursing like it’s her first language. Not like a politician, but like a gangster.
EDGE: So having lived through these two characters, Maggie Lockwood and Nerese Campbell, what do you think you’d be if you weren’t acting?
MB: [Laughs] A gangsta nurse.